Brain Tumor Treatment: A Comparative Guide to Surgery and Radiation Therapy
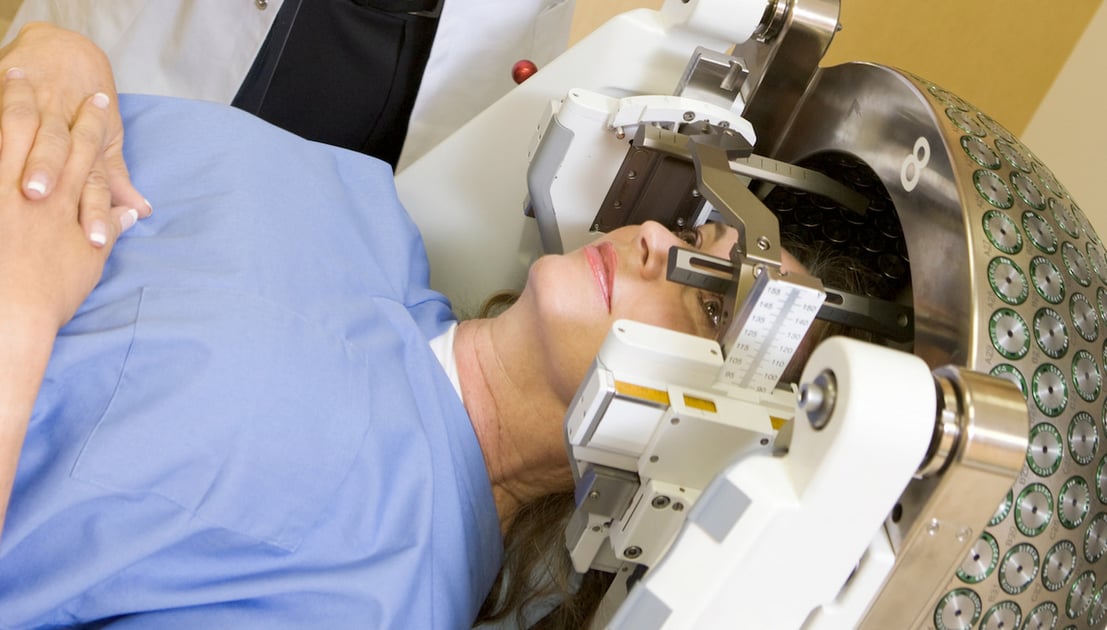
Quick Summary: Surgery is typically favored for accessible tumors requiring immediate pressure relief (debulking). Radiation (such as Gamma Knife) is often the preferred choice for deep-seated or inoperable lesions where surgical risk is high. In many 2026 treatment protocols, both are used in sequence.
When you are first diagnosed with a brain tumor, the sheer amount of information can be paralyzing. Most patients find themselves at a crossroads: Surgery or Radiation? While both are powerful tools, the 'right' choice isn't just about the tumor. It's about your specific anatomy, your symptoms, and your long-term quality of life.
Brain tumors vary widely in behavior and impact. Some tumors require immediate removal to reduce pressure on the brain. Others respond better to targeted radiation over time. Doctors evaluate risks, benefits, and expected outcomes before recommending a treatment plan.
Understanding the difference between surgery and radiation therapy helps patients and families participate in informed discussions. Clear knowledge reduces anxiety and supports realistic expectations during treatment planning.
What Is Brain Tumor Surgery?
Brain tumor surgery involves removing part or all of a tumor through a surgical procedure. Neurosurgeons aim to remove as much tumor tissue as safely possible while protecting normal brain function.
- Purpose of Surgery: Surgery helps reduce intracranial pressure. Tumor removal can relieve symptoms such as headaches, seizures, or weakness. Surgery also provides tissue samples for accurate diagnosis.
- How Surgeons Perform the Procedure: Neurosurgeons use imaging guidance and microsurgical tools during surgery. Advanced techniques help improve precision near sensitive brain areas. Careful planning reduces risk to the surrounding tissue.
- Situations Where Surgery Helps Most: Doctors recommend surgery when tumors remain accessible and clearly defined. Removal often benefits patients with large tumors or mass effect. Surgery also helps when doctors need tissue confirmation.
- Immediate Outcomes After Surgery: Many patients experience symptom relief after tumor removal. Recovery depends on tumor location and the extent of surgery. Doctors monitor neurological function closely after surgery.
What Is Radiation Therapy for Brain Tumors?
Radiation therapy treats brain tumors by using high-energy rays to damage tumor cells and limit their growth. Doctors often use radiation when surgery cannot remove the tumor completely or safely.
- Purpose of Radiation Therapy: Radiation aims to control tumor growth and reduce symptoms. The treatment targets cancer cells while limiting damage to healthy brain tissue. Doctors often use radiation to prevent tumor progression.
- How Radiation Therapy Works: Radiation damages the DNA of tumor cells. Damaged cells lose the ability to grow and divide. Over time, the tumor may shrink or stop growing.
- Types of Radiation Used for Brain Tumors: Doctors may use external beam radiation or highly focused techniques such as stereotactic radiation. Focused methods allow precise targeting. Precision reduces exposure to surrounding brain tissue.
- Treatment Schedule and Duration: Radiation therapy usually occurs over several sessions. Sessions may continue for weeks, depending on tumor type and treatment goals. Doctors plan schedules carefully to balance effectiveness and safety.
Radiation therapy is most effective for specific tumor types and locations. Doctors evaluate suitability before recommending treatment.
When Is Radiation Therapy Preferred Over Surgery for Brain Tumors?
Doctors recommend radiation therapy over surgery in certain clinical situations. Tumor characteristics and patient health guide this decision.
- Tumors in Sensitive or Deep Brain Areas: Some tumors lie close to critical brain structures. Surgery may carry a high neurological risk. Radiation allows treatment without direct surgical intervention.
- Residual Tumor After Surgery: Surgery may not safely remove all tumor tissue. Radiation helps control the remaining tumor cells. Combined treatment improves long-term control.
- Patients Not Suitable for Surgery: Some patients are not suitable for surgery due to age or medical conditions. Radiation provides a non-surgical treatment option. Doctors adjust therapy to the patient's tolerance.
- Slow-Growing or Diffuse Tumors: Certain tumors spread across brain tissue rather than forming a single mass. Radiation helps manage these tumors effectively. Surgery may not offer complete benefit in such cases.
- Tumor Recurrence After Initial Treatment: Radiation often plays a role when tumors return after surgery. Targeted radiation helps control regrowth. Doctors tailor treatment plans carefully.
When Do Doctors Recommend Surgery for Brain Tumors?
Doctors recommend surgery when tumor removal offers a clear clinical benefit and acceptable risk. Several medical factors guide this decision.
- Accessible Tumor Location: Tumors located in areas that surgeons can reach safely often qualify for surgery. Clear access reduces neurological risk. Surgical removal becomes more effective in such cases.
- Large Tumors Causing Pressure: Some tumors increase intracranial pressure. Pressure can cause headaches, vision problems, or weakness. Surgery helps relieve pressure quickly.
- Need for Tissue Diagnosis: Doctors often need tumor tissue to confirm diagnosis and plan treatment. Surgery provides tissue samples for accurate classification. Precise diagnosis supports targeted therapy.
- Rapid Symptom Progression: Worsening symptoms may require urgent intervention. Surgery can reduce tumor burden promptly. Faster relief supports neurological stability.
- Potential for Significant Tumor Removal: Doctors aim to remove as much tumor as safely possible. Greater removal often improves symptom control. Surgical benefit depends on tumor boundaries and location.
Surgery vs Radiation Therapy for Brain Tumor: Key Differences
Surgery and radiation therapy treat brain tumors in different ways. Understanding these differences helps patients compare options realistically.
- Treatment Approach: Surgery removes tumor tissue directly. Radiation therapy targets tumor cells gradually. Each method works through a distinct mechanism.
- Speed of Symptom Relief: Surgery often provides faster symptom relief. Radiation effects develop over time. Timing influences treatment selection.
- Treatment Duration: Surgery involves a single procedure with a recovery time. Radiation therapy requires multiple treatment sessions. Duration varies by protocol.
- Recovery Experience: Surgery requires hospital recovery and healing. Radiation usually allows outpatient treatment. Recovery experience differs for each option.
- Impact on Daily Life: Surgery may limit activity during early recovery. Radiation allows daily routines between sessions. Lifestyle impact varies by patient.
- Risk Profile: Surgery carries risks of surgical and neurological complications. Radiation carries delayed side effects over time. Doctors balance risks carefully.
How Do Doctors Decide Between Surgery and Radiation Therapy for a Brain Tumor?
Doctors do not choose between surgery and radiation therapy based on preference. They base the decision on how the tumor behaves inside the brain and how treatment may affect long-term function.
- The first factor doctors consider is tumor location. Tumors located near critical brain areas that control speech, movement, or vision often carry a higher surgical risk. In such cases, radiation therapy may offer safer control without disturbing essential brain tissue.
- Doctors also assess tumor size and growth pattern. Large tumors that cause pressure or swelling often require surgery to relieve symptoms quickly. Smaller or slowly growing tumors may respond well to radiation without immediate removal.
- Tumor type also plays a major role. Some tumors respond strongly to radiation, while others require surgical removal to reduce tumor burden. Doctors rely on imaging and, when available, tissue diagnosis to guide treatment choice.
- Patient health matters just as much as tumor features. Age, overall fitness, and existing medical conditions influence tolerance to treatment. Some patients tolerate surgery well, while others benefit more from non-surgical approaches.
Can Surgery and Radiation Therapy Be Used Together for Brain Tumor Treatment?
Yes, doctors often use surgery and radiation therapy together as part of a planned treatment sequence. Combined treatment allows doctors to manage the tumor more effectively while balancing safety.
- Surgery often comes first when tumor removal can reduce pressure or symptoms. After surgery, radiation therapy may target remaining tumor cells that surgeons could not remove safely. This approach helps lower the risk of tumor regrowth.
- In some situations, doctors use radiation first to shrink a tumor. Reduced tumor size may make later surgery safer or less invasive. This strategy works especially well for tumors near sensitive brain areas.
- Combined treatment also helps in aggressive or recurrent tumors. Surgery reduces tumor burden, while radiation controls microscopic disease. Doctors tailor the sequence carefully to reduce side effects and protect brain function.
Not every patient requires both treatments. Doctors recommend combined therapy only when the benefits outweigh the risks. Careful planning ensures treatment remains effective without unnecessary exposure.
What Are the Risks and Side Effects of Surgery and Radiation Therapy for Brain Tumors?
Every brain tumor treatment carries some risk, and doctors weigh these risks carefully before recommending surgery or radiation therapy. The goal is always to control the tumor while protecting brain function.
- Brain tumor surgery carries risks related to operating on delicate brain tissue. Patients may experience temporary weakness, speech difficulty, or coordination issues after surgery. These effects often improve with time and rehabilitation, especially when surgery avoids critical brain regions. Infection, bleeding, or swelling may also occur, which is why doctors monitor patients closely after surgery.
- Radiation therapy does not involve an operation, but it can still cause side effects. Fatigue remains common during and after radiation treatment. Some patients notice headaches, skin irritation, or hair loss in the treated area. Radiation effects usually develop gradually rather than immediately.
Long-term effects depend on radiation dose, treatment area, and patient age. Doctors plan radiation carefully to reduce the impact on healthy brain tissue. Follow-up care helps detect and manage delayed effects early.
How Do Recovery and Quality of Life Compare After Surgery and Radiation Therapy?
Recovery experience differs between surgery and radiation therapy, and each path affects daily life in different ways.
- Recovery after brain tumor surgery usually begins in the hospital. Patients may need days or weeks to regain strength, balance, or speech, depending on tumor location and the extent of surgery. Rehabilitation therapy often supports recovery and helps patients gradually return to independence.
- Radiation therapy usually allows patients to remain active during treatment. Many patients continue daily routines while attending scheduled sessions. Fatigue may increase over time, but recovery often feels less intense compared to surgery.
- Quality of life depends on symptom control and neurological function. Surgery may offer faster relief from pressure-related symptoms such as headaches or vision problems. Radiation therapy focuses more on long-term tumor control and stability.
- Doctors consider both physical recovery and mental well-being when planning treatment. The chosen approach aims to preserve independence, cognitive function, and daily comfort as much as possible.
Each patient's recovery journey remains unique. Ongoing support and follow-up play an important role in maintaining quality of life after treatment.
How Do International Patients Plan Brain Tumor Treatment Decisions?
International patients usually start planning after a detailed medical review. Doctors study scans, reports, and symptoms to recommend surgery, radiation therapy, or a combined approach.
Treatment choice also affects travel and stay planning. Surgery often requires a longer stay for recovery and early follow-up. Radiation therapy may involve several weeks of scheduled sessions.
Doctors explain expected timelines clearly before treatment begins. Clear timelines help patients plan accommodation, recovery support, and return travel without pressure.
Recovery needs vary between patients. Some patients need rehabilitation after surgery. Others require monitoring after radiation therapy. Understanding recovery needs early reduces uncertainty.
Next Steps
Surgery and radiation therapy treat brain tumors in different ways. Doctors choose treatment based on tumor features and patient health, not preference. Understanding both options helps patients approach treatment decisions calmly. Clear information reduces fear and supports realistic expectations.
Patients considering brain tumor treatment benefit from expert medical review and personalized planning. Professional guidance helps patients move forward with clarity and confidence.
Hôpitaux connexes
Découvrez les hôpitaux et les centres médicaux liés à ce sujet pour les services de santé de qualité.

Hôpital Medical Park Bahcelievler
L'hôpital Medical Park Bahcelievler est un hôpital accrédité JCI de 242 lits à Istanbul, créé en 2007. Réparti sur 33 000 mètres carrés et 19 étages, ...
Accréditations

Installations

Hôpital super spécialisé BLK-Max, New Delhi
L'hôpital super spécialisé BLK-Max de New Delhi est l'un des principaux établissements de santé de l'Inde, offrant 650 lits, 22 salles d'opération ava...
Accréditations


Installations

Institut de recherche Fortis Memorial (FMRI), Gurgaon
Le Fortis Memorial Research Institute (FMRI), Gurgaon, est un hôpital multi-spécialités de classe mondiale créé en 2013. L'hôpital propose 330 lits, 1...
Accréditations


Installations

Hôpital Artémis, Gurgaon
L'hôpital Artemis de Gurgaon est un hôpital multispécialisé accrédité JCI qui a été créé en 2007. Il offre plus de 750 lits et une infrastructure de c...
Accréditations



Installations

Kokilaben Dhirubhai Ambani Hospital, Mumbai
L'hôpital Kokilaben Dhirubhai Ambani de Mumbai est un hôpital de soins quaternaires accrédité JCI, NABH, NABL et CAP, créé en 2009. Avec 750 lits, 180...
Accréditations



Installations

Hôpitaux Medicover, Hitech City, Hyderabad
Medicover Hospitals, Hitech City, Hyderabad, est un hôpital superspécialisé de 400 lits accrédité par le NABH, créé en 2011. Il fait partie de Medicov...
Accréditations


Installations
Médecins connexes
Connectez-vous avec des médecins expérimentés et des médecins spécialistes dans ce domaine.

Dr Indranil Khan
Consultant

Dr Chandramohan K.
Senior Consultant

Dr Bhavin Visariya
Consultant

Dr Suraj Chiraniya
Senior Consultant

Dr Ninad Katdare
Consultant

Dr Ankit Mahuvakar
Consultant
Articles connexes
Explorez plus d'articles et d'informations sur des sujets de santé similaires.
Back Pain or Something More? When Does a Spine Tumor Require Surgery?

Combien de temps peut-on vivre après une greffe d’organe ?
Qui peut bénéficier d’une greffe d’organe en Inde ? Règles d'éligibilité expliquées
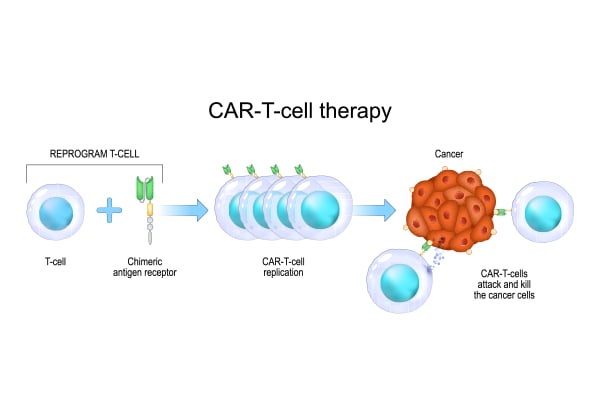
Greffe de moelle osseuse ou thérapie cellulaire CAR-T : quel est le meilleur traitement pour le cancer du sang ?
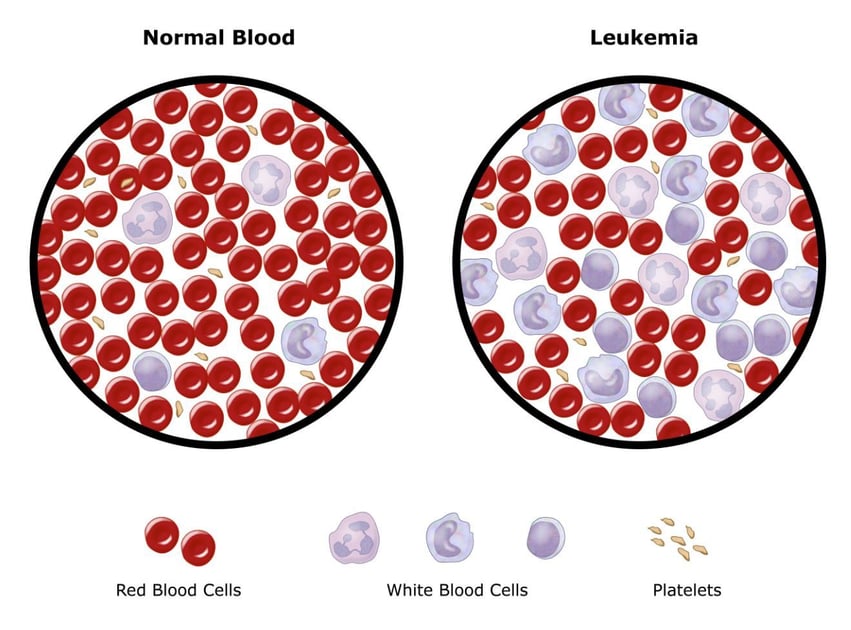
Pouvez-vous survivre à la leucémie sans greffe de moelle osseuse ?
La greffe de moelle osseuse en vaut-elle la peine ? Un guide financier et médical pour les patients internationaux en Inde
Auteur
Afficher tousLe Dr Deepanshu Siwach est un pharmacien clinicien expérimenté titulaire d'un doctorat en pharmacie. Il a plus de 4 ans d'expérience et a travaillé avec des milliers de patients. Il a été associé à ... En savoir plus
Notre site Web utilise des cookies. politique de confidentialité.

