Matibabu ya Saratani ya Larynx Cost in India
Kuhusu Matibabu ya Saratani ya Larynx
Around the world, larynx cancer affects thousands of people each year. More than 183,000 new cases are diagnosed annually, and the condition is more common in individuals who smoke, drink alcohol regularly, or have long-term exposure to harmful chemicals. Recent studies also show a rising link between larynx cancer and certain strains of HPV.
Early diagnosis is critical because symptoms often begin subtly, such as mild hoarseness, and may be overlooked.
Advances in modern oncology (laser surgery, organ-preserving radiation therapy, targeted treatment, and immunotherapy) have significantly improved outcomes. Many patients benefit from treatments that preserve the voice or restore speech through rehabilitation. With timely medical care, larynx cancer can be managed effectively, helping patients regain comfort, function, and confidence.
What Is Larynx Cancer?
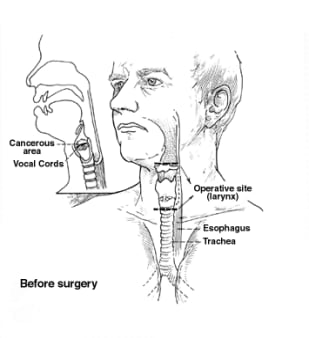
Larynx cancer is a disease in which abnormal cells grow in the voice box, a structure located in the throat that helps produce sound, control airflow, and protect the windpipe during swallowing. Most cases begin in the squamous cells that line the inside of the larynx.
The larynx has three main regions, and cancer can start in any of them:
- Supraglottic Region: This is the upper part of the larynx, located above the vocal cords. Tumors here may spread early to nearby lymph nodes.
- Glottic Region: This area includes the vocal cords. Glottic cancer is often detected early because even small tumors can cause hoarseness.
- Subglottic Region: This is the lower part of the larynx, just below the vocal cords. Tumors here are less common and may grow silently for longer.
Cancer in the larynx can spread to nearby lymph nodes, deeper throat tissues, or distant organs if left untreated. Early diagnosis plays a key role in preserving the voice and improving long-term outcomes.
What Are the Symptoms of Larynx Cancer?
Larynx cancer often begins with subtle voice changes or throat discomfort. Because these symptoms can resemble common throat infections, many people ignore them in the early stages. Recognizing the warning signs helps ensure timely diagnosis and better treatment outcomes.
Early Symptoms
- Persistent hoarseness lasting more than two weeks
- Voice changes such as roughness, weakness, or pitch alteration
- A constant sore throat or feeling of irritation
- Dry cough that does not settle
- Difficulty projecting the voice
Advanced Symptoms
- Pain or difficulty while swallowing
- A lump or swelling in the neck
- Ear pain on one side
- Breathing difficulty or noisy breathing
- Unexplained weight loss
- Frequent choking episodes
- Blood-tinged saliva or coughing up small amounts of blood
When to Seek a Doctor
A person should consult a specialist if hoarseness or throat discomfort does not improve with routine treatment, especially in smokers or people exposed to alcohol or irritants. Early detection improves the chances of preserving the voice and achieving better outcomes.
How Is Larynx Cancer Diagnosed?
Doctors use several tests to confirm larynx cancer, assess the tumor's location, and determine how far it has spread. Accurate diagnosis helps create a personalized treatment plan that aims to preserve function and improve long-term outcomes.
- Laryngoscopy: A thin, flexible tube with a camera is sent through the nose or mouth to examine the vocal cords and surrounding structures. It is often the first and most crucial test.
- Biopsy: During laryngoscopy, the doctor may remove a small tissue sample for lab analysis. A biopsy confirms whether cancer cells are present.
- CT Scan or MRI: These imaging tests show the tumor's size and whether it has invaded nearby tissues, cartilage, or lymph nodes.
- PET-CT Scan: PET-CT helps identify active cancer cells throughout the body and detects spread to distant organs.
- Ultrasound of the Neck: This test evaluates lymph nodes and helps determine if they require biopsy or surgical removal.
- Chest X-Ray: Doctors may use this to check whether the cancer/tumor has spread to the lungs.
Staging Evaluation
After all tests, the doctor assigns a stage from I to IV based on tumor size, lymph node involvement, and distant spread. Staging guides the choice of surgery, radiation, chemotherapy, or combined treatments.
Accurate diagnosis ensures larynx cancer patients receive the most effective treatment with the best chance of preserving voice and breathing function.
What Are the Latest Treatment Options for Larynx Cancer?
Doctors treat larynx cancer using a combination of surgery, radiation, chemotherapy, and modern targeted therapies. The treatment plan depends on the cancer's stage, location, and whether preserving the voice is possible. Early-stage cancers often respond well to single-modality treatment, while advanced cases may require a combination approach.
- Laser Surgery: Laser surgery helps remove small, early-stage tumors with minimal damage to surrounding tissues. It is often used for glottic cancers and may preserve normal voice quality.
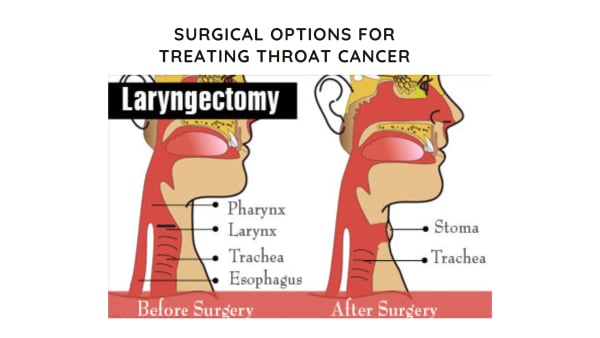
- Partial Laryngectomy: In this procedure, doctors remove only the affected portion of the larynx. It helps preserve speech and swallowing functions while removing cancerous tissue.
- Total Laryngectomy: When cancer is advanced or involves multiple regions, surgeons may remove the entire larynx. Patients breathe through a permanent opening in the neck (stoma) and later learn voice rehabilitation techniques.
- Radiation Therapy: Radiation uses high-energy beams to destroy cancer cells. It works effectively in early-stage cancers and is often combined with chemotherapy for more advanced tumors. Techniques such as IMRT and IGRT help precisely target the cancer.
- Chemotherapy: Doctors use chemotherapy to shrink tumors, enhance the effect of radiation, or treat cancer that has spread. It is commonly combined with radiation when surgery is not the first choice.
- Chemoradiation: This combination treatment preserves the larynx in many cases by shrinking the tumor enough to avoid the need for surgery.
- Targeted Therapy: Drugs like cetuximab block specific proteins that help cancer cells grow. They may be used alongside radiation or chemotherapy.
- Immunotherapy: Medications such as pembrolizumab or nivolumab help the immune system recognize and destroy cancer cells. They are helpful in recurrent or metastatic larynx cancer.
- Voice Rehabilitation: After surgery, especially total laryngectomy, speech therapists teach patients alternative speaking methods, including voice prosthesis or esophageal speech.
Treatment plans aim to remove the cancer, preserve essential functions, and improve long-term quality of life.
Pata mpango wa matibabu ya bure
About Matibabu ya Saratani ya Larynx in India
Gharama ya Matibabu ya Saratani ya Larynx nchini India ni nini?
Gharama ya matibabu ya saratani ya larynx nchini India kwa ujumla ni kati ya$3,000 hadi $15,000(takriban₹2.5 laki hadi ₹12.5 laki) Bei ya mwisho inategemea hatua ya saratani, mpango wa matibabu, aina ya upasuaji, teknolojia inayotumiwa kwa mionzi, na ikiwa tiba inayolengwa au tiba ya kinga inahitajika.
India inapendekezwa kwa matibabu ya saratani ya larynx kwa sababu inatoa huduma ya juu ya oncology ya kichwa na shingo kwa bei nafuu zaidi ikilinganishwa na nchi nyingi za Magharibi.
Ifuatayo ni muhtasari wa kina wa gharama za matibabu.
Aina ya Matibabu | Gharama ya wastani (USD) | Takriban. Gharama (INR) |
| Upasuaji wa Laser | $2,000 - $4,000 | ₹1.6 - ₹3.3 laki |
| Laryngectomy ya sehemu | $3,500 - $6,000 | ₹2.9 - ₹5 laki |
| Jumla ya Laryngectomy | $4,500 - $7,500 | ₹3.7 - ₹6.2 laki |
| Tiba ya Mionzi (IMRT/IGRT) | $2,500 - $5,000 | ₹2 - ₹4.1 laki |
| Chemotherapy (kwa kila mzunguko) | $250 - $450 | ₹20,000 - ₹36,000 |
| 6–7 Mizunguko ya Kemia | $1,500 - $3,000 | ₹1.2 - ₹2.5 laki |
| Tiba inayolengwa (Cetuximab, nk.) | $1,000 - $2,500 kwa mwezi | ₹80,000 - ₹2 laki |
| Tiba ya kinga (Nivolumab, Pembrolizumab) | $1,500 - $4,000 kwa dozi | ₹1.2 - ₹3.3 laki |
| Prosthesis ya Sauti (ikiwa inahitajika) | $300 - $800 | ₹25,000 - ₹65,000 |
- Ugonjwa wa hatua ya awali hugharimu kidogo kwa sababu matibabu yanaweza kuhusisha tu tiba ya leza au mionzi.
- Ugonjwa wa hatua ya juu unaweza kuhitaji matibabu ya pamoja, na kuongeza gharama ya jumla.
- Dawa zinazolengwa na za kinga huongeza kwa kiasi kikubwa gharama za jumla.
Gharama Inajumuisha Nini
- Ada ya daktari wa upasuaji kwa laryngectomy ya sehemu au jumla
- Gharama za ukumbi wa michezo na ganzi
- Kukaa hospitalini kwa idadi iliyopendekezwa ya siku
- Vipimo vya kawaida vya damu kabla ya upasuaji au mionzi
- Dawa za kawaida wakati wa kulazwa hospitalini
- Vikao vya tiba ya mionzi (ikiwa ni sehemu ya kifurushi)
- Gharama za usimamizi wa chemotherapy
- Ufuatiliaji na utunzaji wa baada ya upasuaji
- Ziara moja ya ufuatiliaji baada ya kutokwa
- Huduma ya uuguzi na msaada wa lishe
Vipengele hivi huunda sehemu muhimu ya vifurushi vingi vya matibabu ya saratani.
Nini Gharama Haijumuishi
- Uchunguzi wa PET-CT na upigaji picha wa hali ya juu
- Dawa za tiba inayolengwa (kama vile cetuximab)
- Dawa za immunotherapy (kama pembrolizumab au nivolumab)
- Vifaa bandia vya sauti na urekebishaji wa hotuba
- Ukaaji wa ziada wa hospitali zaidi ya kifurushi
- Vipimo vya biomarker (hali ya HPV, upimaji wa PD-L1, maelezo mafupi ya kinasaba)
- Udhibiti wa matatizo au hali ya awali ya matibabu
- Vipimo vya ufuatiliaji wa muda mrefu
- Malazi na kusafiri kwa wagonjwa wa kimataifa
Gharama inaweza kutofautiana kidogo kati ya hospitali, kwa hivyo wagonjwa mara nyingi huomba makadirio ya kina kabla ya kuanza matibabu.
Je! Gharama ya Matibabu ya Saratani ya Larynx katika Miji Tofauti ya India ni Gani?
Gharama za matibabu ya saratani ya zoloto hutofautiana katika miji yote ya India kwa sababu ya tofauti za miundombinu ya hospitali, utaalamu wa oncologist, vifaa vya uchunguzi, na ufikiaji wa teknolojia ya juu ya mionzi. Miji ya Metro kawaida huwa na gharama za juu za matibabu, wakati miji ya daraja la 2 hutoa huduma ya kiuchumi zaidi lakini ya kuaminika.
Jedwali hapa chini linatoa ulinganisho wa wazi ili kuwasaidia wagonjwa kupanga matibabu yao kulingana na eneo na bajeti.
Jiji | Gharama ya Wastani ya Matibabu (USD) | Takriban. Gharama (INR) |
| New Delhi | $4,000 - $12,000 | ₹3.3 - ₹10 laki |
| Mumbai | $4,500 - $14,000 | ₹3.7 - ₹11.6 laki |
| Bangalore | $3,800 - $11,000 | ₹3.1 - ₹9 laki |
| Chennai | $3,500 - $10,000 | ₹2.9 - ₹8.3 laki |
| Hyderabad | $3,800 - $11,000 | ₹3.1 - ₹9 laki |
- Delhi na Mumbaikutoa vitengo vya juu vya oncology ya kichwa na shingo vilivyo na teknolojia ya kisasa ya mionzi, ikiwa ni pamoja na IMRT na IGRT.
- Bangalore na Hyderabadkutoa huduma ya kisasa ya saratani kwa bei za ushindani na madaktari bingwa wa upasuaji na matibabu.
- Chennaiinajulikana kwa utaalamu mkubwa wa oncology wa ENT na vifurushi vya matibabu vya gharama nafuu.
Ni Mambo Gani Huathiri Gharama ya Matibabu ya Saratani ya Larynx nchini India?
Sababu kadhaa za matibabu na zisizo za matibabu huathiri jumla ya gharama ya matibabu ya saratani ya larynx nchini India. Kila mgonjwa anahitaji mpango wa matibabu wa kibinafsi kulingana na hatua, eneo la tumor, na afya kwa ujumla, ambayo husababisha kutofautiana kwa bei.
- Hatua ya Saratani:Saratani za hatua za awali zinaweza kuhitaji upasuaji wa laser au mionzi pekee, wakati saratani za hali ya juu mara nyingi zinahitaji upasuaji pamoja na mionzi na chemotherapy, na kuongeza gharama ya jumla.
- Aina ya upasuaji:Laser microsurgery inagharimu kidogo. Laryngectomy ya sehemu ina bei ya wastani. Jumla ya laryngectomy ni ghali zaidi kwa sababu ya ugumu wake, kukaa hospitalini, na utunzaji wa baada ya upasuaji.
- Teknolojia ya Mionzi Inayotumika:IMRT, IGRT, na VMAT hutoa matibabu sahihi lakini yanagharimu zaidi ya mbinu za kawaida za mionzi.
- Mahitaji ya matibabu ya pamoja:Ukaaji wa kemikali au upasuaji unaofuatwa na mionzi huongeza jumla ya muda wa matibabu na gharama ya jumla.
- Tiba inayolengwa na Immunotherapy:Dawa kama vile cetuximab, pembrolizumab na nivolumab huongeza sana gharama za matibabu kutokana na gharama kubwa za kila mzunguko au kwa kila dozi.
- Urekebishaji wa Sauti ya Prosthesis na Urekebishaji:Wagonjwa wanaopitia laryngectomy jumla wanaweza kuhitaji uunganisho wa sauti na tiba ya usemi, ambayo inaweza kuongeza gharama.
- Kitengo cha Hospitali:Hospitali za hali ya juu zilizo na idara za oncology za hali ya juu hutoza ada kubwa kuliko vituo vya masafa ya kati.
- Utaalam wa Oncologist na Upasuaji:Wataalamu wa oncologists wenye ujuzi wa juu wa kichwa na shingo wanaweza malipo zaidi, lakini ujuzi wao unaboresha matokeo ya upasuaji na kupunguza matatizo.
- Muda wa Kukaa Hospitalini:Kulazwa hospitalini kwa muda mrefu kwa sababu ya aina ya upasuaji au hali ya matibabu huongeza gharama zote.
Je, Gharama nchini India Inalinganishwaje na Nchi Nyingine?
Matibabu ya saratani ya larynx nchini India ni nafuu zaidi kuliko katika nchi nyingi za Magharibi na Asia, wakati bado inatoa huduma ya juu ya oncology, mbinu za kisasa za upasuaji, na wataalam waliofunzwa kimataifa. Faida hii ya gharama hufanya India kuwa mahali panapopendelewa kwa wagonjwa wanaotafuta matibabu ya ubora wa juu kwa bei nzuri.
Ifuatayo ni ulinganisho wa wastani wa gharama za matibabu katika maeneo yote ya afya duniani:
Nchi | Gharama ya wastani (USD) |
| Marekani | $30,000 - $80,000 |
| Uingereza | $25,000 - $60,000 |
| Singapore | $20,000 - $45,000 |
| UAE | $18,000 - $40,000 |
| Thailand | $12,000 - $25,000 |
| India | $3,000 - $15,000 |
Wagonjwa kuokoa60% hadi 80%kwa kuchagua India huku bado ikipokea matibabu ya hali ya juu ya saratani, ufikiaji wa teknolojia ya kisasa ya mionzi, na huduma ya upasuaji ya kitaalam. Bei ya India yenye msingi wa thamani na matokeo dhabiti ya kimatibabu yanaifanya kuwa mojawapo ya chaguo la kuaminika zaidi kwa matibabu ya saratani ya zoloto duniani kote.
Je, Kupona Kunaonekanaje Baada ya Matibabu ya Saratani ya Larynx?
Kupona kutokana na matibabu ya saratani ya larynx inategemea hatua ya utambuzi, aina ya matibabu iliyopokelewa, na afya ya jumla ya mgonjwa. Kwa mbinu za kisasa za upasuaji, tiba inayolengwa ya mionzi, na urekebishaji unaofaa, wagonjwa wengi hupata faraja iliyoboreshwa, utendakazi bora, na hali nzuri ya maisha baada ya matibabu.
Ahueni Baada ya Upasuaji
- Upasuaji wa Laser:Wagonjwa kawaida hupona haraka. Sauti inaweza kuboreka ndani ya siku kadhaa hadi wiki, kulingana na kiwango cha kuondolewa kwa tishu.
- Sehemu ya Laryngectomy:Wagonjwa huweka sauti yao ya asili, ingawa inaweza kusikika tofauti. Kumeza kunaboresha kwa kasi kwa wiki chache.
- Jumla ya Laryngectomy:Uokoaji unajumuisha kujifunza njia mpya za kuzungumza kupitia kiungo bandia cha sauti au tiba ya usemi. Kupumua hutokea kwa njia ya ufunguzi katika shingo, na wagonjwa kukabiliana vizuri na mwongozo sahihi.
Kupona Baada ya Tiba ya Mionzi
- Uchovu, ukavu, na usumbufu wa koo ni kawaida lakini ni ya muda.
- Wagonjwa wengi huanza tena kula kawaida na shughuli za kila siku ndani ya wiki chache baada ya kumaliza matibabu.
- Sauti kawaida huboresha mionzi inapotumiwa kwa saratani ya glottic ya hatua za mapema.
Ahueni Wakati wa Chemotherapy na Chemoradiation
- Madhara yanaweza kujumuisha kichefuchefu, uchovu, na usumbufu mdogo wa kumeza.
- Dawa za usaidizi husaidia wagonjwa kuvumilia matibabu vizuri.
- Tiba ya pamoja mara nyingi huepuka haja ya laryngectomy jumla katika kesi zilizochaguliwa.
Je, ni kiwango gani cha Mafanikio ya Matibabu ya Saratani ya Larynx?
Mafanikio hutegemea hatua ya saratani:
- Awamu ya awali (Hatua ya I-II):Viwango vya juu vya tiba, mara nyingi hapo juu80-90%, hasa wakati wa kutibiwa kwa upasuaji wa laser au tiba ya mionzi.
- Ubora wa ndani (Hatua ya III):Tiba ya pamoja (kemoradiation au upasuaji wa sehemu) hupata udhibiti unaofaa kwa wagonjwa wengi.
- Hatua ya Juu (Hatua ya IV):Matibabu hulenga kudhibiti, kupunguza dalili, na kuongeza muda wa kuishi kwa upasuaji, chemotherapy, tiba ya kinga, au tiba inayolengwa.
Kwa matibabu sahihi na ukarabati, wagonjwa wengi hurudi kwenye taratibu za kila siku za maana na kurejesha imani katika sauti na mawasiliano yao.
Kwa nini unapaswa kuchagua India kwa Matibabu ya Saratani ya Larynx?
India imekuwa nchi inayoongoza kwa matibabu ya saratani ya zoloto kwa sababu inatoa huduma ya matibabu ya hali ya juu, teknolojia ya hali ya juu ya saratani na wataalam wenye uzoefu mkubwa kwa gharama ndogo ya kimataifa. Wagonjwa hunufaika kutokana na utunzaji unaotegemewa na matokeo dhabiti ya kliniki bila muda mrefu wa kungojea.
- Madaktari bingwa wa magonjwa ya kichwa na shingo:India ina madaktari bingwa wa upasuaji wa ENT, wataalam wa magonjwa ya kichwa na shingo, na wataalam wa mionzi ambao hushughulikia idadi kubwa ya visa vya saratani ya larynx. Utaalam wao unasaidia utambuzi sahihi, upasuaji wa kuhifadhi sauti, na matokeo bora ya kuishi.
- Teknolojia ya Juu ya Mionzi:Hospitali hutumia teknolojia za kisasa kama vile IMRT, IGRT, VMAT, na viongeza kasi vya mstari ili kulenga uvimbe huku wakilinda tishu zenye afya. Njia hizi husaidia kuhifadhi kazi za kumeza na hotuba wakati wowote iwezekanavyo.
- Usaidizi wa Nguvu wa Kurekebisha Sauti na Usemi:Madaktari maalumu wa tiba ya usemi huwasaidia wagonjwa kurejesha sauti zao baada ya laryngectomy sehemu au jumla. Chaguo za bandia za sauti zinapatikana pia kwa urejeshaji wa hotuba ya muda mrefu.
- Utunzaji Jumuishi wa Saratani Chini ya Paa Moja:Picha za uchunguzi, vitengo vya upasuaji, oncology ya matibabu, ukarabati, na huduma za usaidizi hufanya kazi pamoja katika kituo kimoja, kuhakikisha uratibu usio na mshono katika mchakato wote wa matibabu.
- Vipindi Vifupi vya Kusubiri:Wagonjwa wanaweza kuanza matibabu haraka, faida muhimu kwa saratani zinazoendelea haraka au kusababisha shida ya kupumua na sauti.
- Msaada wa Kimataifa wa Wagonjwa:Hospitali hutoa usaidizi wa visa ya matibabu, uhamisho wa uwanja wa ndege, wakalimani wa lugha, mipango ya malazi, na ufuatiliaji usio na mshono, na kufanya matibabu yasiwe na mafadhaiko kwa wagonjwa wa kimataifa.
Matibabu ya Saratani ya Larynx kulinganisha gharama na nchi
Linganisha Matibabu ya Saratani ya Larynx gharama katika nchi tofauti kufanya uamuzi sahihi juu ya matibabu yako.
| Nchi | Anuwai ya gharama (USD) | Akiba inayowezekana | Hatua |
|---|---|---|---|
INIndiaSasaThamani bora | $3,000 - $15,000 | — | Pata nukuu |
Kumbuka: Gharama zinaweza kutofautiana kulingana na uchaguzi wa hospitali, aina ya chumba, huduma za ziada, na mahitaji ya matibabu ya mtu binafsi.
Hospitali zinazoongoza kwa Matibabu ya Saratani ya Larynx katika India

Medical Park Bahcelievler Hospital
Medical Park Bahcelievler Hospital is a 242-bed JCI-accredited hospital in Istanbul, established in 2007. Spread across 33,000 square meters and 19 fl...
Vibali

Vifaa

Memorial Ankara Hospital
Memorial Ankara Hospital is a JCI-accredited private hospital in Turkey, with more than 230 beds and 60 intensive care units. Spread across 42,000 squ...
Vibali

Vifaa
Saudi German Hospital, Cairo
Saudi German Hospital, Cairo, is a multi-specialty hospital located in Cairo and part of the Saudi German Hospitals Group. Established in 2016, it has...
Vibali

Vifaa
Cleopatra Hospital, Cairo
Cleopatra Hospital is a 356-bed private hospital in Cairo, Egypt, established in 1984 and part of the Cleopatra Hospitals Group. It offers more than 4...
Vifaa

As-Salam International Hospital, Cairo
As-Salam International Hospital is a 300+ bed JCI-accredited hospital in Cairo, Egypt. It offers advanced care in cardiology, oncology, neurology, ort...
Vibali


Vifaa

Piyavate Hospital
Piyavate Hospital is a 150-bed private hospital in central Bangkok, established in 1993. The hospital provides care in cardiology, neurology, orthoped...
Vibali


Vifaa
Phyathai 2 International Hospital
Phyathai 2 International Hospital is a JCI-accredited tertiary care hospital in Bangkok, Thailand, established in 1987. The hospital operates 550 inpa...
Vibali


Vifaa

Bangpakok 9 International Hospital
Bangpakok 9 International Hospital is a JCI-accredited tertiary care hospital in Bangkok, Thailand, established in 2003. Operating under the BPK Hospi...
Vibali


Vifaa

Vejthani Hospital
Vejthani Hospital is a JCI-accredited tertiary care hospital in Bangkok, Thailand, established in 1994. With approximately 263 inpatient beds and more...
Vibali

Vifaa

Bangkok Hospital
Bangkok Hospital is one of Thailand's leading private tertiary care hospitals, established in 1972 and operating under the BDMS network. The hospital ...
Vibali

Vifaa
Taratibu zinazofanana
Matunzio

Maswali
Mhakiki
Tazama ZoteDr. Priya Tiwari is a renowned medical oncologist trained at the prestigious All India Institute of Medical Sciences (AIIMS). She specializes in comprehensive cancer care and is committed to deliver... Soma zaidi
Mwandishi
Tazama Zote
Mkuu - Huduma za Wagonjwa wa Kimataifa
Dk. Riya Shree ni mtaalamu wa tiba ya mwili ambaye alimaliza mafunzo yake katika Hospitali ya Mata Chanan Devi, New Delhi, akipata uzoefu wa kuhudumia wagonjwa na urekebishaji. Alihudumu kwenye mstar... Soma zaidi
Vinjari na Idara
Chunguza taratibu katika idara tofauti
Taratibu zinazohusiana
Taratibu zingine katika idara hii
Pata mpango wa matibabu ya bure
Tovuti yetu hutumia kuki. Sera ya faragha.

