Chirurgie de l'épilepsie Cost in India
À propos Chirurgie de l'épilepsie
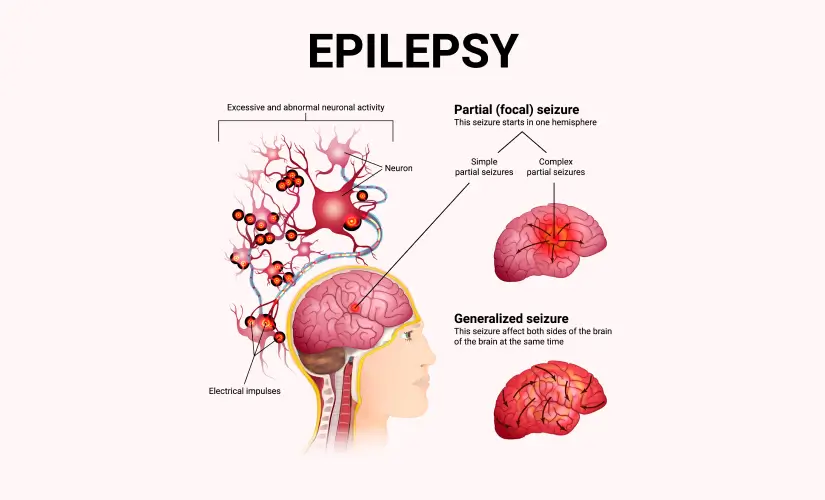
What Is Epilepsy?
Epilepsy is a chronic disorder that causes a person to experience repeated, unprovoked seizures. These seizures happen due to sudden, abnormal bursts of electrical activity in the brain that interrupt normal brain function. While the exact cause isn't always known, epilepsy can result from brain injury, infections, stroke, tumors, or genetic conditions.
Seizures in epilepsy can vary widely. Some may cause a person to fall, shake uncontrollably, or lose consciousness. Others may be more subtle, such as brief moments of staring, confusion, or unusual sensations. For a diagnosis of epilepsy, a person must have had at least two unprovoked seizures that were not caused by temporary triggers like fever or low blood sugar.
Epilepsy affects people of all ages, but it often begins in childhood or later adulthood. With the right treatment protocol, most people with epilepsy can manage their condition effectively. Treatment typically starts with medications, but when drugs fail to control the seizures (especially after trying two or more types), doctors may consider surgery or device-based therapies.
Modern advances in neuroimaging and brain mapping have enabled the precise localization of seizure origins in the brain, facilitating highly targeted surgical procedures. For many patients with drug-resistant epilepsy, especially those with focal seizures, surgery offers a real chance at long-term seizure control and a better quality of life.
What Is Epilepsy Surgery?
Epilepsy surgery is a specialized medical procedure designed to help people whose seizures do not improve with medication alone. Doctors usually consider surgery when a person has drug-resistant epilepsy, meaning they've tried multiple anti-seizure medicines without success. The goal of the surgery is to either remove or disconnect the part of the brain where the seizures begin, giving the patient a better chance at leading a seizure-free life.
There are different types of epilepsy surgeries, and the choice depends on where the seizures originate and how they affect the brain. For instance, if seizures arise from a small, specific area that does not control vital functions such as speech or movement, that part may be safely removed. In other cases, doctors may perform a disconnective surgery to interrupt the abnormal signals in the brain without removing any tissue.
Unlike medications that only control seizures, surgery aims to eliminate or significantly reduce seizure activity at the source. It is not a first-line treatment, but for many patients, especially those who've suffered for years, it offers a path toward better health, independence, and overall quality of life.
What are the Different Types of Epilepsy Surgery?
Epilepsy surgery includes a range of specialized procedures designed to treat seizures. The type of surgery chosen depends on the origin of the seizures in the brain, their severity, and the patient's overall health condition. These procedures are typically performed by experienced neurosurgeons and supported by technologies such as brain imaging, intraoperative monitoring, and, in some centers, robotic assistance.
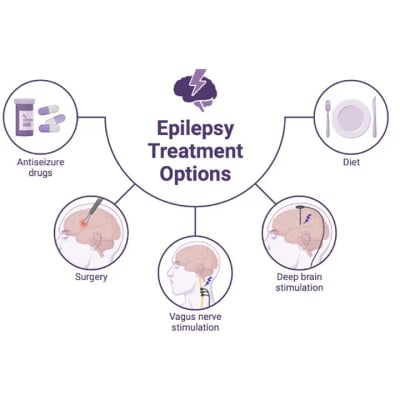
A few of the most common types of epilepsy surgeries performed worldwide are:
- Temporal Lobectomy: Temporal lobectomy is one of the most widely performed epilepsy surgeries worldwide. Surgeons remove a portion of the temporal lobe where seizures begin, usually in patients with mesial temporal lobe epilepsy (MTLE). This type of surgery has one of the highest success rates, with up to 70–80% of patients achieving long-term seizure freedom. It is particularly effective for adults and older children who have focal seizures originating from this area.
- Lesionectomy: A lesionectomy targets a clearly identifiable lesion on brain scans, such as a tumor, cavernoma, or cortical dysplasia, that is responsible for triggering seizures. The surgeon removes only the lesion and a small margin of surrounding brain tissue. This procedure is considered highly effective when the lesion is the sole cause of seizures, and it minimizes the risk of affecting normal brain functions.
- Corpus Callosotomy: This is a disconnective surgery where the corpus callosum (a bundle of nerve fibers connecting the two halves of the brain) is partially or fully severed. It is typically performed in children with severe generalized seizures, especially drop attacks or tonic seizures that result in frequent falls and injuries. While corpus callosotomy may not completely stop seizures, it often reduces their severity and frequency, offering a safer life for the patient.
- Hemispherectomy or Hemispherotomy: Used primarily in young children with widespread seizures confined to one hemisphere of the brain, this surgery involves either removing or disconnecting one side of the brain. Conditions like Rasmussen's encephalitis or extensive cortical malformations may require this procedure. Despite its complexity, many children experience dramatic improvements in seizure control and development afterward, with the remaining hemisphere adapting over time.
- Multiple Subpial Transections (MST): When the seizure focus lies near an essential part of the brain (such as the speech or motor area) and cannot be removed, MST offers a safer option. In this technique, surgeons make tiny cuts (transections) in the brain's outer layer to disrupt seizure pathways without removing any tissue. It's less commonly used but can be effective in select cases.
- Laser Ablation Surgery (Stereotactic Laser Thermoablation): Some advanced neurology centers now offer minimally invasive laser ablation for epilepsy. The procedure involves inserting a thin laser fiber into the seizure focus and destroying the tissue using heat. The benefits include a shorter hospital stay, faster recovery, and minimal scarring. It is best suited for patients with small, well-defined seizure foci.
- Vagus Nerve Stimulation (VNS): Although not strictly surgical in the traditional sense, VNS involves implanting a device under the skin of the chest area that sends electrical pulses to the vagus nerve, helping reduce seizure frequency. It is often used when brain surgery is not an option.
Who Needs Epilepsy Surgery?
Not every person with epilepsy will need surgery, but for some, it becomes the best option after other treatments fail.
- Patients with Drug-Resistant Epilepsy: The primary candidates for epilepsy surgery are people who have drug-resistant epilepsy (DRE). It means they continue to experience seizures even after trying at least two appropriate anti-seizure medications at the correct doses and for a reasonable duration. Studies show that the chances of becoming seizure-free drop significantly after two failed medications, which is why surgery becomes a viable alternative at this stage.
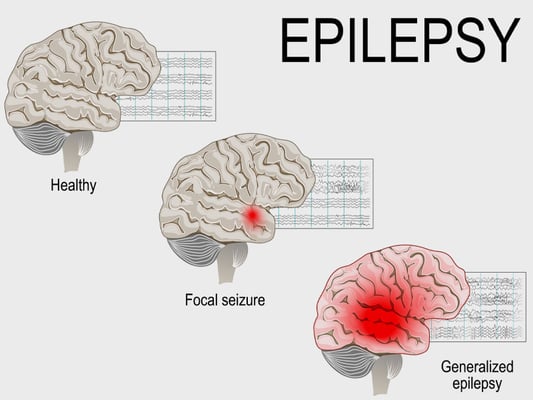
- People with Focal Seizures: Surgery works best when seizures start from a specific area of the brain, often referred to as the seizure focus. These are known as focal or partial seizures, and they may or may not spread to other areas of the brain. If doctors can pinpoint the source of the seizure through EEG monitoring, MRI, or other imaging tests, surgery becomes a strong option.
- Patients Whose Seizures Affect Daily Life: Some individuals experience seizures that severely interfere with their daily activities, such as walking, working, attending school, or even maintaining personal safety. Frequent seizures can lead to social isolation, mental health issues, and injuries from falls or accidents. When medications do not help and quality of life suffers, doctors may recommend surgery to control the seizures and restore independence.
- Children with Developmental Risk Due to Seizures: In children, uncontrolled seizures can negatively affect brain development, learning ability, and behavior. Pediatric neurologists in India often recommend surgery early for children with severe epilepsy to protect cognitive function and promote better long-term outcomes. In such cases, early surgical intervention can lead to developmental catch-up and improved quality of life.
- Patients at Risk of SUDEP: People with frequent generalized tonic-clonic seizures may be at higher risk of sudden unexpected death in epilepsy (SUDEP). Reducing or eliminating seizures through surgery can significantly lower this risk. For some patients, this becomes a life-saving decision.
- Candidates Identified Through Pre-Surgical Evaluation: Before recommending surgery, hospitals in India conduct an in-depth pre-surgical evaluation, which includes continuous video EEG monitoring, MRI and PET scans, neuropsychological testing, and functional mapping (for speech, movement, and memory). Only those whose seizure origin is clearly identified and who meet safety criteria are selected for surgery.
What are the Benefits of Epilepsy Surgery?
Epilepsy surgery offers hope to individuals whose seizures remain uncontrolled despite taking multiple medications. For many of these patients, surgery can lead to life-changing improvements.
- Seizure Reduction or Elimination: The most immediate and noticeable benefit is a significant decrease in seizure frequency, and in many cases, complete seizure freedom. Depending on the type of surgery and location of the seizure focus, up to 70–80% of patients may stop having seizures altogether after surgery.
- Improved Quality of Life: When seizures become less frequent or disappear entirely, patients often find that their daily life improves dramatically. They may regain independence, return to school or work, drive again (depending on local laws), and engage more fully in social and family activities.
- Fewer or Lower Doses of Medications: Many people with epilepsy take multiple anti-seizure drugs, often leading to side effects such as fatigue, memory problems, dizziness, and mood changes. After successful surgery, some patients are able to reduce the number of medications they take or even discontinue them altogether under medical supervision.
- Cognitive and Developmental Gains in Children: Children with uncontrolled epilepsy may suffer from delayed speech, poor academic performance, and behavioral problems due to repeated seizures and medication side effects. Surgery at an appropriate age can not only reduce seizures but also improve cognitive development, learning abilities, and social interaction.
- Enhanced Emotional and Mental Health: Living with frequent seizures can cause depression, anxiety, and isolation. Many patients report feeling more optimistic and confident after surgery, especially if their seizures stop or become less frequent.
- Long-Term Stability: With appropriate post-operative care and follow-up, the results of epilepsy surgery can be long-lasting. Many patients remain seizure-free or well-controlled for years or even decades after surgery.
What are the Side Effects of Epilepsy Surgery
While epilepsy surgery offers significant benefits, like seizure reduction and improved quality of life, it is still a brain surgery, and like any surgery, it carries some risks.
- Temporary Confusion or Fatigue: After surgery, especially during the first few days, patients often experience confusion, fatigue, or drowsiness.
- Memory or Language Difficulties: Depending on the area of the brain that is affected, some individuals may experience temporary or mild issues with memory, language, or concentration.
- Weakness or Numbness: In rare cases, surgery can cause weakness, tingling, or numbness on one side of the body if motor areas of the brain are affected.
- Vision or Sensory Changes: Some patients report visual disturbances or changes in their field of vision after surgery, especially when surgery involves the occipital or temporal lobes.
- Mood and Emotional Shifts: Mood changes such as depression, anxiety, or irritability may occur temporarily after surgery. These shifts can result from changes in brain chemistry, the stress of surgery, or adjusting to a new life without seizures.
- Surgical Risks: As with any surgery, there are standard medical risks, including infection, bleeding, or reactions to anesthesia.
Recovery Timeline After Epilepsy Surgery
Recovering from epilepsy surgery is a step-by-step process that involves physical healing, mental adjustment, and ongoing medical care. While every patient's experience is slightly different, there is a general timeline most people follow. Recovery typically spans several weeks to months, depending on the type of epilepsy surgery performed and the individual's overall health.
Immediate Post-Surgery Period (0–1 Week)
After the surgery, patients usually spend a few hours in the recovery room before being transferred to a monitored hospital ward or ICU, especially if the procedure was complex. During this phase, doctors closely monitor brain function, vital signs, and the surgical site's healing progress. Mild headaches, swelling, or fatigue are common, and pain is controlled with medication.
Most epilepsy patients remain in the hospital for approximately 5 to 7 days, although more extensive procedures, such as hemispherectomy, may require a slightly more extended stay. During this time, patients begin gentle movement and are evaluated by neurologists and rehabilitation teams.
Early Recovery Phase (2–6 Weeks)
After discharge, patients continue their recovery at home or in a short-term rehabilitation center. They may still feel tired or mentally foggy, especially in the first couple of weeks. Doctors schedule follow-up visits to monitor progress, remove stitches or staples as necessary, and adjust medications as needed.
During this phase, doctors activate or fine-tune any implanted devices (like a VNS) and review seizure activity. Many patients notice a reduction in seizures soon after surgery, though full benefits may take time to appear. Light daily activities can usually resume within 2–3 weeks, but tasks requiring concentration may take longer.
Rehabilitation and Adjustment (1–3 Months)
Depending on the type of surgery, patients may require occupational therapy, physical therapy, or speech therapy. These services help improve strength, coordination, memory, and language if any deficits occurred during surgery.
Patients are also carefully monitored for emotional changes, as this is a time of mental adjustment. Some people feel a surge of confidence after gaining seizure control, while others experience anxiety about returning to everyday life.
Long-Term Recovery and Follow-Up (3 Months and Beyond)
By the three-month mark, most patients have resumed many of their everyday routines. Those who were seizure-free post-surgery often begin tapering off medications under their neurologist's guidance, though this process can take many months.
Regular follow-ups are conducted for at least one to two years to monitor brain health, medication levels, and cognitive function. In some cases, further evaluations are done if seizures persist or return.
Patients who respond well to surgery can often return to driving, working, and socializing, enjoying a better quality of life than before.
Obtenez un plan de traitement gratuit
About Chirurgie de l'épilepsie in India
Quel est le coût de la chirurgie de l’épilepsie en Inde ?
Le coût de la chirurgie de l'épilepsie en Inde est plus abordable que dans de nombreux pays occidentaux, tout en maintenant des normes élevées de sécurité et de résultats cliniques. Les patients internationaux choisissent souvent l’Inde pour des soins neurochirurgicaux avancés à une fraction des frais facturés aux États-Unis, au Royaume-Uni ou en Europe.
Le coût de la chirurgie de l'épilepsie en Inde varie de4 000 $ à 9 000 $,en fonction de plusieurs facteurs, dont le type d'intervention chirurgicale, l'infrastructure hospitalière, l'expertise du chirurgien et la durée du séjour à l'hôpital. Voici une répartition générale par type de chirurgie :
- Le coût d'unlobectomie temporaleen Inde va de5 000 $ à 7 000 $, en fonction de l'hôpital et de la complexité de l'intervention chirurgicale.
- UNlésionectomiecoûte généralement entre4 000 $ et 6 000 $, surtout lorsque la lésion est clairement définie et facilement accessible.
- Pour les patients subissant uncallosotomie corporelle, le coût se situe dans la fourchette de6 000 $ à 8 000 $.
- UNhémisphèrectomie ou hémiphérotomie, étant une intervention chirurgicale plus étendue et plus complexe, son prix se situe entre7 000 $ et 9 000 $.
- Chirurgie d'ablation au laser, lorsqu'il est disponible, coûte généralement entre6 500 $ et 9 000 $, offrant une alternative peu invasive.
- Le coût destimulation du nerf vague (VNS), y compris le prix du dispositif implanté, varie généralement de8 000 $ à 12 000 $.
Ces forfaits comprennent généralement :
- Examens préopératoires (IRM, EEG, tests neuropsychologiques)
- Procédure chirurgicale et anesthésie
- Séjour à l'hôpital (généralement 5 à 10 jours)
- Surveillance en soins intensifs (si nécessaire)
- Médicaments pendant l'admission
- Soins postopératoires et suivi précoce
Coût par rapport à d’autres pays
Les patients de pays comme les États-Unis, le Canada, le Royaume-Uni et l'Australie font souvent face à des coûts allant de30 000 $ à 70 000 $ou plus pour des procédures similaires. Cela fait de l’Inde une option attrayante pour les familles qui recherchent des soins spécialisés sans fardeau financier.
Quels facteurs affectent le coût de la chirurgie de l’épilepsie en Inde ?
Le coût global de la chirurgie de l'épilepsie en Inde varie d'un patient à l'autre en fonction de plusieurs facteurs médicaux et logistiques. Bien que les honoraires chirurgicaux de base puissent être similaires dans tous les hôpitaux, des éléments spécifiques liés à l'état du patient, aux besoins de traitement et aux préférences de l'hôpital influencent souvent le coût final.
- Type de chirurgie pratiquée :La variation de coût la plus importante vient du type de chirurgie de l’épilepsie pratiquée. Par exemple, une lobectomie temporale est généralement plus abordable qu’une hémisphèrectomie ou une procédure de stimulation du nerf vague (VNS), qui implique un dispositif implantable.
- Choix de l'hôpital et de la ville :Les frais chirurgicaux diffèrent souvent selon la ville et l'hôpital. Les hôpitaux des villes métropolitaines comme Mumbai ou Bangalore peuvent facturer plus que ceux des petites villes.
- Expérience du chirurgien et expertise de l'équipe :Les neurochirurgiens très expérimentés et les équipes complètes de chirurgie de l'épilepsie exigent généralement des honoraires plus élevés, ce qui peut se refléter dans le coût total du traitement.
- Tests préchirurgicaux et imagerie :Avant la chirurgie, les patients subissent une évaluation détaillée qui peut inclure des analyses IRM, une surveillance vidéo EEG, des analyses TEP ou SPECT et des évaluations neuropsychologiques. Le nombre et la complexité de ces tests peuvent avoir un impact significatif sur le coût total du traitement.
- Durée du séjour à l’hôpital et des soins en soins intensifs :Certains patients peuvent nécessiter un séjour hospitalier plus prolongé, en particulier ceux qui subissent des procédures complexes ou qui connaissent des complications post-chirurgicales.
- Type de chambre et d'hébergement :Les chambres privées, les suites de luxe et les équipements destinés aux patients, tels que le séjour d'un compagnon ou des repas personnalisés, peuvent également avoir un impact sur le coût total.
- Récupération post-chirurgicale et médicaments :Les premières semaines après la chirurgie peuvent nécessiter des examens de suivi, des médicaments et une rééducation physique ou cognitive.
Pourquoi choisir l’Inde pour la chirurgie de l’épilepsie ?
L’Inde est une plaque tournante mondiale pour la chirurgie de l’épilepsie, grâce à sa combinaison unique d’expertise médicale, d’infrastructures modernes et de prix abordables. Des patients du monde entier se rendent chaque année en Inde à la recherche de soins neurologiques avancés, à la fois de haute qualité et rentables.
- Neurochirurgiens de classe mondiale avec une formation mondiale :L’Inde abrite un nombre croissant de neurochirurgiens hautement qualifiés spécialisés dans la chirurgie de l’épilepsie. Ils apportent des années d’expérience dans le traitement de cas d’épilepsie complexes, tant chez les adultes que chez les enfants, et maîtrisent toutes les procédures pertinentes.
- Technologie avancée et outils de diagnostic :Les principaux hôpitaux indiens sont équipés des dernières technologies nécessaires à une chirurgie de l'épilepsie sûre et précise. Ceux-ci incluent l'IRM haute résolution, la surveillance vidéo EEG, les scans TEP et SPECT, les systèmes de neuronavigation et la cartographie cérébrale peropératoire.
- Des taux de réussite élevés comparables à ceux de l’Occident :Les hôpitaux indiens signalent systématiquement des taux d’absence de crises de 60 à 80 %, en fonction de la procédure et du profil du patient. En plus de la réduction des crises, de nombreux patients bénéficient d’améliorations significatives en termes de clarté mentale, de mobilité, de bien-être émotionnel et de qualité de vie globale.
- Forfaits de traitement rentables :L’une des raisons les plus convaincantes de choisir l’Inde est le coût considérablement inférieur du traitement. Les chirurgies de l'épilepsie en Inde peuvent coûter 60 à 80 % moins cher que dans les pays occidentaux, sans compromettre la qualité.
- Soins multilingues et sensibles à la culture :Les hôpitaux indiens offrent un environnement chaleureux et inclusif aux patients internationaux. De nombreuses institutions mettent à disposition des interprètes, un personnel multilingue et des soins adaptés à la culture, garantissant ainsi que les patients et leurs familles se sentent compris et respectés.
- Pas de listes d'attente et processus rationalisé :Contrairement à de nombreux pays où les systèmes de santé publics impliquent de longs délais d’attente, la chirurgie de l’épilepsie en Inde est programmée rapidement. Une fois le diagnostic confirmé et les évaluations pré-chirurgicales terminées, la plupart des patients subissent une intervention chirurgicale en quelques jours.
Services pour les patients internationaux
Les meilleurs hôpitaux indiens et animateurs de tourisme médical ont développé des services spécialisés pour rendre la chirurgie de l'épilepsie accessible et sans stress pour les patients voyageant de l'étranger. À partir du moment où un patient exprime son intérêt jusqu'à longtemps après l'intervention chirurgicale, le système est conçu pour offrir confort, clarté et commodité à chaque étape.
- Assistance pour visa médical :Les hôpitaux délivrent souvent une lettre d'invitation pour un visa, ce qui aide les patients à obtenir rapidement un visa médical. Dans de nombreux cas, le traitement des visas est accéléré pour les personnes qui suivent des traitements neurologiques, en particulier si les crises sont fréquentes ou altèrent leur vie.
- Prise en charge à l'aéroport et transport local :La plupart des grands hôpitaux proposent des services de prise en charge à l'aéroport pour garantir que les patients arrivent confortablement et en toute sécurité. Le transport local est également organisé pour les visites de suivi, les tests de diagnostic et la sortie.
- Hébergement et repas abordables :Les patients peuvent choisir parmi une gamme d’hébergements à proximité, notamment des maisons d’hôtes et des hôtels de luxe. Les services de repas sont adaptés aux besoins alimentaires, y compris des options végétariennes, halal ou adaptées aux diabétiques.
- Services d'interprétation linguistique :La communication est cruciale pendant le traitement. C'est pourquoi les meilleurs hôpitaux fournissent des interprètes parlant couramment l'arabe, le français, l'espagnol, le russe, le swahili et bien plus encore, selon la région du patient.
- Coordinateurs de patients internationaux dédiés :Chaque patient international se voit attribuer un coordinateur qui agit comme point de contact unique tout au long du parcours médical. Le coordinateur aide à l'admission à l'hôpital, aux rendez-vous, à la facturation, à la préparation des documents et à la planification des sorties.
- Soins de suivi :Les hôpitaux planifient souvent des téléconsultations après le retour du patient chez lui pour vérifier les progrès de sa guérison, gérer ses médicaments et répondre à ses éventuelles préoccupations.
- Prise en charge des déplacements et de la documentation :Les coordinateurs de patients aident avec le change de devises, les lettres d'assurance, les extensions de visa et les certificats de condition physique de retour à domicile.
Comparaison des Coûts de Chirurgie de l'épilepsie par Pays
Comparez les coûts de Chirurgie de l'épilepsie dans différents pays pour prendre une décision éclairée concernant votre traitement médical.
| Pays | Fourchette de Coût (USD) | Économies Potentielles | Action |
|---|---|---|---|
INIndiaActuelMeilleure Valeur | $4,000 - $9,000 | — | Obtenir un Devis |
Note : Les coûts peuvent varier selon le choix de l'hôpital, le type de chambre, les services supplémentaires et les exigences médicales individuelles. Contactez-nous pour un devis personnalisé.
Hôpitaux Leaders pour Chirurgie de l'épilepsie en India

BLK-Max Super Speciality Hospital, New Delhi
BLK-Max Super Speciality Hospital in New Delhi is one of India's premier healthcare institutions, offering 650 beds, 22 advanced operation theatres, a...
Accréditations


Installations

Fortis Memorial Research Institute (FMRI), Gurgaon
Fortis Memorial Research Institute (FMRI), Gurgaon, is a world-class multi-specialty hospital established in 2013. The hospital offers 330 beds, 15 op...
Accréditations


Installations

Artemis Hospital, Gurgaon
Artemis Hospital, Gurgaon, is a JCI accredited multispecialty hospital that was established in 2007. It offers 750+ beds and world -class infrastructu...
Accréditations



Installations

Kokilaben Dhirubhai Ambani Hospital, Mumbai
Kokilaben Dhirubhai Ambani Hospital, Mumbai, is a JCI, NABH, NABL, and CAP-accredited quaternary care hospital established in 2009. With 750 beds, 180...
Accréditations



Installations

Medicover Hospitals, Hitech City, Hyderabad
Medicover Hospitals, Hitech City, Hyderabad, is a 400-bed NABH-accredited super-specialty hospital established in 2011. It is part of Medicover, a glo...
Accréditations


Installations
SP Medifort Hospital
SP Medifort, Thiruvananthapuram, is a JCI-accredited, 475-bed multi-super-specialty hospital spread across 500,000 sq. ft. The hospital houses 10 modu...
Accréditations


Installations
Gleneagles Global Health City, Chennai
Gleneagles Global Health City, Chennai, is a 200-bed quaternary-care hospital and part of the IHH Healthcare network, one of the world’s largest priva...
Accréditations

Installations
MIOT International, Chennai
MIOT International, Chennai, is a 1,000-bed NABH- and NABL-accredited multispecialty hospital serving patients from more than 130 countries. Establish...
Accréditations

Installations
Paras Hospital, Gurgaon
Paras Hospital, Gurgaon, established in 2006, is a 300-bed NABH- and NABL-accredited tertiary care hospital offering over 36 super specialties. The ho...
Accréditations

Installations
Shalby Sanar International Hospital, Gurgaon
Shalby Sanar International Hospital, Gurgaon, is a 150-bed NABH-accredited multispecialty hospital offering advanced care in oncology, cardiology, org...
Accréditations



Installations
Procédures Similaires
Galerie

FAQ
Critique
Afficher tousDr. SK Rajan is an internationally trained and AO-certified Spine Surgeon with extensive expertise in managing complex spinal disorders. He has trained at leading national and global institutions, i... En savoir plus
Auteur
Afficher tousLe Dr Deepanshu Siwach est un pharmacien clinicien expérimenté titulaire d'un doctorat en pharmacie. Il a plus de 4 ans d'expérience et a travaillé avec des milliers de patients. Il a été associé à ... En savoir plus
Parcourir par Département
Explorer les procédures dans différents départements
Procédures Associées
Autres procédures de ce département
Obtenez un plan de traitement gratuit
Notre site Web utilise des cookies. politique de confidentialité.







