Cirurgia de Epilepsia Custo em Índia
Sobre Cirurgia de Epilepsia
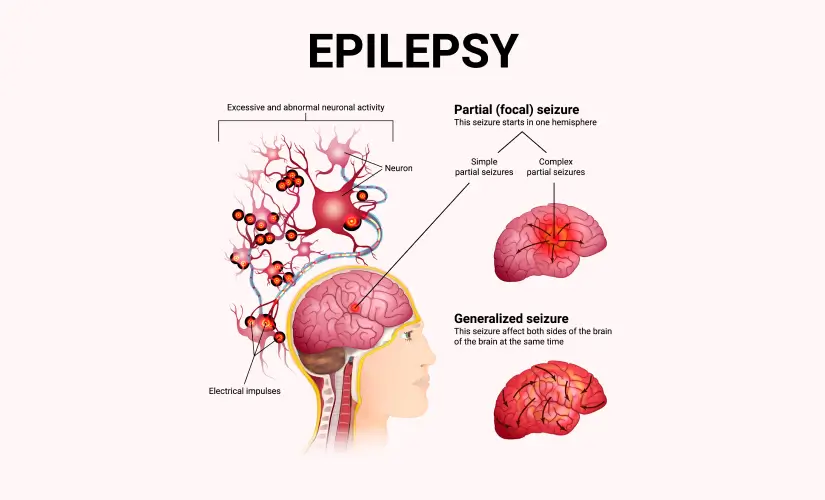
O que é epilepsia?
A epilepsia é uma doença crônica que faz com que a pessoa experimenteConvulsões repetidas e não provocadas. Essas convulsões acontecem devido a rajadas súbitas e anormais de atividade elétrica no cérebro que interrompem a função normal do cérebro. Embora a causa exata nem sempre seja conhecida, a epilepsia pode resultar de lesões cerebrais, infecções, derrame, tumores ou condições genéticas.
As convulsões na epilepsia podem variar muito. Alguns podem causar uma queda de uma pessoa, tremer incontrolavelmente ou perder a consciência. Outros podem ser mais sutis, como breves momentos de olhares, confusão ou sensações incomuns. Para o diagnóstico de epilepsia, uma pessoa deve ter tidoPelo menos duas convulsões não provocadasIsso não foi causado por gatilhos temporários, como febre ou baixo nível de açúcar no sangue.
A epilepsia afeta pessoas de todas as idades, mas geralmente começa na infância ou na idade adulta. Com o protocolo de tratamento correto, a maioria das pessoas com epilepsia pode gerenciar sua condição de forma eficaz. O tratamento normalmente começa com medicamentos, mas quando os medicamentos não conseguem controlar as convulsões (especialmente após tentar dois ou mais tipos), os médicos podem considerar a cirurgia ou terapias baseadas em dispositivos.
Os avanços modernos em neuroimagem e mapeamento cerebral permitiram a localização precisa das origens das convulsões no cérebro, facilitandoProcedimentos cirúrgicos altamente direciona. Para muitos pacientes com epilepsia resistente a medicamentos, especialmente aqueles com convulsões focais, a cirurgia oferece uma chance real de controle de convulsões a longo prazo e uma melhor qualidade de vida.
O que é cirurgia de epilepsia?
A cirurgia de epilepsia é um procedimento médico especializado projetado para ajudar pessoas cujas convulsões não melhoram apenas com a medicação. Os médicos geralmente consideram a cirurgia quando uma pessoaEpilepsia resistente a medicamentos, o que significa que eles tentaram vários medicamentos anticonvulsivantes sem sucesso. O objetivo da cirurgia é remover ou desconectar a parte do cérebro onde as convulsões começam, dando ao paciente uma chance melhor de levar uma vida livre de convulsões.
Existem diferentes tipos de cirurgias de epilepsia, e a escolha depende de onde as convulsões se originam e como elas afetam o cérebro. Por exemplo, se surgirem convulsões de uma área pequena e específica que não controla funções vitais, como fala ou movimento, essa parte pode ser removida com segurança. Em outros casos, os médicos podem realizar uma cirurgia desconectada para interromper os sinais anormais no cérebro sem remover nenhum tecido.
Ao contrário dos medicamentos que controlam apenas as convulsões, a cirurgia visaElimine ou reduza significativamente a atividade de convulsões na fonte. Não é um tratamento de primeira linha, mas para muitos pacientes, especialmente aqueles que sofrem há anos, oferece um caminho para uma melhor saúde, independência e qualidade de vida geral.
Quais são os diferentes tipos de cirurgia de epilepsia?
A cirurgia de epilepsia inclui uma série de procedimentos especializados projetados para tratar convulsões. O tipo de cirurgia escolhida depende da origem das convulsões no cérebro, sua gravidade e condição geral de saúde do paciente. Esses procedimentos são normalmente realizados por neurocirurgiões experientes e apoiados por tecnologias como imagens cerebrais, monitoramento intraoperatório e, em alguns centros, assistência robótica.
Alguns dos tipos mais comuns de cirurgias de epilepsia realizados em todo o mundo são:
- Lobectomia temporal:A lobectomia temporal é uma das cirurgias de epilepsia mais amplamente realizadas em todo o mundo. Os cirurgiões removem uma parte do lobo temporal onde começam as convulsões, geralmente em pacientes com epilepsia do lobo temporal mesial (TLE). Esse tipo de cirurgia tem uma das maiores taxas de sucesso, com até 70 a 80% dos pacientes alcançando a liberdade de convulsões a longo prazo. É particularmente eficaz para adultos e crianças mais velhas que têm convulsões focais oriundas dessa área.
- Lesionectomia:A lesionectomia tem como alvo uma lesão claramente identificável em exames cerebrais, como tumor, cavernoma ou displasia cortical, que é responsável por desencadear convulsões. O cirurgião remove apenas a lesão e uma pequena margem do tecido cerebral circundante. Esse procedimento é considerado altamente eficaz quando a lesão é a única causa de convulsões e minimiza o risco de afetar as funções normais do cérebro.
- Calosotomia do corpo:Esta é uma cirurgia desconexo onde o corpo caloso (um feixe de fibras nervosas conectando as duas metades do cérebro) é parcial ou totalmente cortado. É normalmente realizado em crianças com convulsões generalizadas graves, especialmente ataques de gota ou convulsões tônicas que resultam em quedas frequentes e lesões. Embora a calosotomia de corpus possa não interromper completamente as convulsões, geralmente reduz sua gravidade e frequência, oferecendo uma vida mais segura para o paciente.
- Hemisferectomia ou hemisferotomia:Usada principalmente em crianças pequenas com convulsões generalizadas confinadas a um hemisfério do cérebro, esta cirurgia envolve remover ou desconectar um lado do cérebro. Condições como encefalite de Rasmussen ou malformações corticais extensas podem exigir esse procedimento. Apesar de sua complexidade, muitas crianças experimentam melhorias dramáticas no controle e desenvolvimento das convulsões depois, com o hemisfério restante se adaptando ao longo do tempo.
- Múltiplas transecções subpiais (MST):Quando o foco da convulsão se encontra próximo de uma parte essencial do cérebro (como fala ou área motora) e não pode ser removido, o MST oferece uma opção mais segura. Nesta técnica, os cirurgiões fazem pequenos cortes (transecções) na camada externa do cérebro para interromper as vias de convulsões sem remover nenhum tecido. É menos comumente usado, mas pode ser eficaz em casos selecionados.
- Cirurgia de ablação a laser (termoablação estereotáxica a laser):Alguns centros de neurologia avançados agora oferecem ablação a laser minimamente invasiva para epilepsia. O procedimento envolve a inserção de uma fina fibra de laser no foco da convulsão e destruindo o tecido usando o calor. Os benefícios incluem uma estadia mais curta no hospital, uma recuperação mais rápida e um mínimo de cicatrizes. É mais adequado para pacientes com focos de convulsões pequenos e bem definidos.
- Estimulação do nervo vago (VNS):Embora não seja estritamente cirúrgico no sentido tradicional, o VNS envolve a implantação de um dispositivo sob a pele da área do tórax que envia pulsos elétricos para o nervo vago, ajudando a reduzir a frequência de convulsões. É frequentemente usado quando a cirurgia no cérebro não é uma opção.
Quem precisa de cirurgia de epilepsia?
Nem todas as pessoas com epilepsia precisam de cirurgia, mas para alguns, ela se torna a melhor opção após a falha de outros tratamentos.
- Pacientes com epilepsia resistente a medicamentos:Os principais candidatos à cirurgia de epilepsia são pessoas que apresentam epilepsia resistente a medicamentos (DRE). Isso significa que eles continuam a ter convulsões, mesmo depois de tentar pelo menos dois medicamentos anticonvulsivos apropriados nas doses corretas e por um período razoável. Estudos mostram que as chances de se tornarem livres de convulsões caem significativamente após dois medicamentos com falha, razão pela qual a cirurgia se torna uma alternativa viável nesta fase.
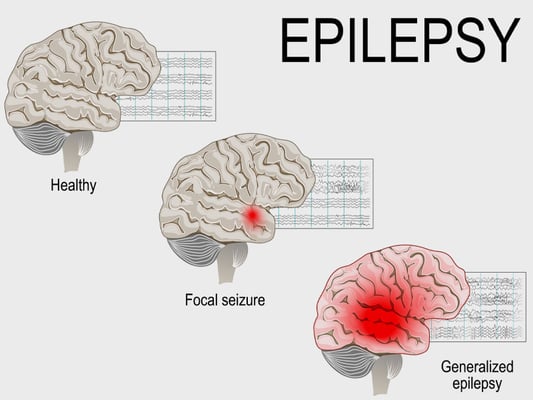
- Pessoas com convulsões focais:A cirurgia funciona melhor quando as convulsões começam em uma área específica do cérebro, muitas vezes referida como o foco da convulsão. Estes são conhecidos como convulsões focais ou parciais, e podem ou não se espalhar para outras áreas do cérebro. Se os médicos podem identificar a origem da convulsão por meio de monitoramento de EEG, ressonância magnética ou outros exames de imagem, a cirurgia se torna uma opção forte.
- Pacientes cujas convulsões afetam a vida diária:Algumas pessoas experimentam convulsões que interferem severamente em suas atividades diárias, como caminhar, trabalhar, frequentar a escola ou até mesmo manter a segurança pessoal. Convulsões frequentes podem levar ao isolamento social, problemas de saúde mental e lesões por quedas ou acidentes. Quando os medicamentos não ajudam e a qualidade de vida sofre, os médicos podem recomendar uma cirurgia para controlar as convulsões e restaurar a independência.
- Crianças com risco de desenvolvimento devido a convulsões:Em crianças, convulsões descontroladas podem afetar negativamente o desenvolvimento do cérebro, a capacidade de aprendizado e o comportamento. Os neurologistas pediátricos na Índia geralmente recomendam a cirurgia no início de crianças com epilepsia grave para proteger a função cognitiva e promover melhores resultados a longo prazo. Nesses casos, a intervenção cirúrgica precoce pode levar a um desenvolvimento do desenvolvimento e à melhoria da qualidade de vida.
- Pacientes com risco de SUDEP:Pessoas com convulsões tônico-clônicas generalizadas frequentes podem ter maior risco de morte súbita e inesperada na epilepsia (SUDEP). Reduzir ou eliminar convulsões por meio de cirurgia pode diminuir significativamente esse risco. Para alguns pacientes, isso se torna uma decisão que salva vidas.
- Candidatos identificados por meio de avaliação pré-cirúrgica:Antes de recomendar a cirurgia, os hospitais na Índia realizam uma avaliação pré-cirúrgica em profundidade, que inclui monitoramento contínuo de EEG por vídeo, ressonância magnética e PET, testes neuropsicológicos e mapeamento funcional (para fala, movimento e memória). Somente aqueles cuja origem convulsiva está claramente identificada e que atendem aos critérios de segurança são selecionados para cirurgia.
Quais são os benefícios da cirurgia de epilepsia?
A cirurgia de epilepsia oferece esperança a indivíduos cujas convulsões permanecem descontroladas, apesar de tomarem vários medicamentos. Para muitos desses pacientes, a cirurgia pode levar a melhorias na mudança de vida.
- Redução ou eliminação de apreensões:O benefício mais imediato e perceptível é uma diminuição significativa na frequência de convulsões e, em muitos casos, a liberdade total da convulsão. Dependendo do tipo de cirurgia e do local do foco das convulsões, até 70 a 80% dos pacientes podem parar de ter convulsões após a cirurgia.
- Melhor qualidade de vida:Quando as convulsões se tornam menos frequentes ou desaparecem completamente, os pacientes geralmente descobrem que sua vida diária melhora drasticamente. Eles podem recuperar a independência, voltar à escola ou trabalhar, dirigir novamente (dependendo das leis locais) e se envolver mais plenamente em atividades sociais e familiares.
- Menos ou menos doses de medicamentos:Muitas pessoas com epilepsia tomam vários medicamentos anticonvulsivos, muitas vezes levando a efeitos colaterais, como fadiga, problemas de memória, tonturas e alterações de humor. Após uma cirurgia bem sucedida, alguns pacientes são capazes de reduzir o número de medicamentos que tomam ou até mesmo descontinuá-los sob supervisão médica.
- Ganhos cognitivos e de desenvolvimento em crianças:Crianças com epilepsia não controlada podem sofrer de fala tardia, desempenho acadêmico ruim e problemas comportamentais devido a convulsões repetidas e efeitos colaterais de medicamentos. A cirurgia em uma idade adequada pode não apenas reduzir as convulsões, mas também melhorar o desenvolvimento cognitivo, as habilidades de aprendizagem e a interação social.
- Saúde emocional e mental aprimorada:Viver com convulsões frequentes pode causar depressão, ansiedade e isolamento. Muitos pacientes relatam sentir-se mais otimistas e confiantes após a cirurgia, especialmente se suas convulsões pararem ou se tornarem menos frequentes.
- Estabilidade a longo prazo:Com cuidados e acompanhamento adequados no pós-operatório, os resultados da cirurgia de epilepsia podem ser duradouros. Muitos pacientes permanecem livres de convulsões ou bem controlados por anos ou mesmo décadas após a cirurgia.
Quais são os efeitos colaterais da cirurgia de epilepsia
Embora a cirurgia de epilepsia ofereça benefícios significativos, como redução de convulsões e qualidade de vida melhorada, ainda é uma cirurgia no cérebro e, como qualquer cirurgia, acarreta alguns riscos.
- Confusão temporária ou fadiga:Após a cirurgia, especialmente durante os primeiros dias, os pacientes geralmente apresentam confusão, fadiga ou sonolência.
- Dificuldades de memória ou linguagem:Dependendo da área do cérebro afetada, alguns indivíduos podem ter problemas temporários ou leves com memória, linguagem ou concentração.
- Fraqueza ou dormência:Em casos raros, a cirurgia pode causar fraqueza, formigamento ou dormência em um lado do corpo se as áreas motoras do cérebro forem afetadas.
- Visão ou alterações sensoriais:Alguns pacientes relatam distúrbios visuais ou alterações em seu campo de visão após a cirurgia, especialmente quando a cirurgia envolve os lobos occipitais ou temporais.
- Mudanças emocionais e de humor:Alterações de humor, como depressão, ansiedade ou irritabilidade, podem ocorrer temporariamente após a cirurgia. Essas mudanças podem resultar de mudanças na química do cérebro, do estresse da cirurgia ou do ajuste a uma nova vida sem convulsões.
- Riscos cirúrgicoComo em qualquer cirurgia, existem riscos médicos padrão, incluindo infecção, sangramento ou reações à anestesia.
Recuperação do tempo após a cirurgia de epilepsia
A recuperação da cirurgia de epilepsia é um processo passo a passo que envolve a cura física, o ajuste mental e o cuidado médico contínuo. Embora a experiência de cada paciente seja um pouco diferente, há uma linha do tempo geral que a maioria das pessoas segue. A recuperação normalmente se estende por várias semanas a meses, dependendo do tipo de cirurgia de epilepsia realizada e da saúde geral do indivíduo.
Período imediato pós-operatório (0–1 semana)
Após a cirurgia, os pacientes geralmente passam algumas horas na sala de recuperação antes de serem transferidos para uma enfermaria ou UTI monitorada, especialmente se o procedimento for complexo. Durante esta fase, os médicos monitoram de perto a função cerebral, os sinais vitais e o progresso de cura do local cirúrgico. Dores de cabeça leves, inchaço ou fadiga são comuns, e a dor é controlada com medicamentos.
A maioria dos pacientes com epilepsia permanece no hospital por aproximadamente5 a 7 dias, embora procedimentos mais extensos, como hemisferectomia, possam exigir uma permanência um pouco mais prolongada. Durante esse período, os pacientes iniciam um movimento suave e são avaliados por neurologistas e equipes de reabilitação.
Fase de recuperação precoce (2–6 semanas)
Após a alta, os pacientes continuam sua recuperação em casa ou em um centro de reabilitação de curto prazo. Eles ainda podem se sentir cansados ou mentalmente embaçados, especialmente nas primeiras semanas. Os médicos agendam visitas de acompanhamento para monitorar o progresso, remover pontos ou grampos conforme necessário e ajustar os medicamentos conforme necessário.
Durante essa fase, os médicos ativam ou ajustam os dispositivos implantados (como um VNS) e revisam a atividade de convulsões. Muitos pacientes notam uma redução nas convulsões logo após a cirurgia, embora todos os benefícios possam levar tempo para aparecer. As atividades diárias leves geralmente podem ser retomadas dentro2–3 semanas, mas tarefas que exigem concentração podem demorar mais.
Reabilitação e ajuste (1–3 meses)
Dependendo do tipo de cirurgia, os pacientes podem precisar deTerapia ocupacional, fisioterapia ou fonoaudiologia. Esses serviços ajudam a melhorar a força, a coordenação, a memória e a linguagem se ocorrerem déficits durante a cirurgia.
Os pacientes também são cuidadosamente monitorados quanto a mudanças emocionais, pois este é um momento de ajuste mental. Algumas pessoas sentem uma onda de confiança depois de obter o controle das convulsões, enquanto outras sentem ansiedade em retornar à vida cotidiana.
Recuperação e acompanhamento a longo prazo (3 meses e mais)
Na marca de três meses, a maioria dos pacientes retomou muitas de suas rotinas diárias. Aqueles que estavam sem convulsões após a cirurgia geralmente começam a diminuir os medicamentos sob a orientação de seu neurologista, embora esse processo possa levar muitos meses.
Os acompanhamentos regulares são realizados por pelo menos um a dois anos para monitorar a saúde do cérebro, os níveis de medicação e a função cognitiva. Em alguns casos, outras avaliações são feitas se as convulsões persistirem ou retornarem.
Pacientes que respondem bem à cirurgia podem voltar aCondução, trabalho e convívio, desfrutando de uma qualidade de vida melhor do que antes.
Obtenha um plano de tratamento gratuito
Sobre Cirurgia de Epilepsia em Índia
Qual é o custo da cirurgia de epilepsia na Índia?
O custo da cirurgia de epilepsia na Índia é mais acessível em comparação com muitos países ocidentais, mantendo elevados padrões de segurança e resultados clínicos. Pacientes internacionais muitas vezes escolhem a Índia para cuidados neurocirúrgicos avançados por uma fração das taxas cobradas nos EUA, no Reino Unido ou na Europa.
O custo da cirurgia de epilepsia na Índia varia deUS$ 4.000 a US$ 9.000,dependendo de vários fatores, incluindo o tipo de cirurgia, a infraestrutura hospitalar, a experiência do cirurgião e a duração da internação. Aqui está uma análise geral por tipo de cirurgia:
- O custo de umlobectomia temporalna Índia varia deUS$ 5.000 a US$ 7.000, dependendo do hospital e da complexidade da cirurgia.
- UMlesionectomianormalmente custa entreUS$ 4.000 e US$ 6.000, especialmente quando a lesão é claramente definida e de fácil acesso.
- Para pacientes submetidos acorpo calosotomia, o custo está dentro da faixa deUS$ 6.000 a US$ 8.000.
- UMhemisferectomia ou hemisferotomia, por ser uma cirurgia mais extensa e complexa, tem preço entreUS$ 7.000 e US$ 9.000.
- Cirurgia de ablação a laser, quando disponível, normalmente custa entreUS$ 6.500 e US$ 9.000, fornecendo uma alternativa minimamente invasiva.
- O custo deestimulação do nervo vago (ENV), incluindo o preço do dispositivo implantado, normalmente varia deUS$ 8.000 a US$ 12.000.
Esses pacotes geralmente incluem:
- Investigações pré-operatórias (ressonância magnética, EEG, testes neuropsicológicos)
- Procedimento cirúrgico e anestesia
- Internação hospitalar (normalmente de 5 a 10 dias)
- Monitoramento da UTI (se necessário)
- Medicamentos durante a internação
- Cuidados pós-operatórios e acompanhamento precoce
Custo comparado a outros países
Pacientes de países como os EUA, Canadá, Reino Unido e Austrália muitas vezes enfrentam custos que variam deUS$ 30.000 a US$ 70.000ou mais para procedimentos semelhantes. Isso torna a Índia uma opção atraente para famílias que procuram atendimento especializado sem encargos financeiros.
Quais fatores afetam o custo da cirurgia de epilepsia na Índia?
O custo total da cirurgia de epilepsia na Índia varia de um paciente para outro com base em vários fatores médicos e logísticos. Embora a taxa cirúrgica básica possa ser semelhante entre hospitais, elementos específicos relacionados à condição do paciente, às necessidades de tratamento e às preferências do hospital geralmente influenciam o custo final.
- Tipo de cirurgia realizada:A variação de custo mais significativa vem do tipo de cirurgia de epilepsia realizada. Por exemplo, uma lobectomia temporal é geralmente mais acessível do que uma hemisferectomia ou procedimento de estimulação do nervo vago (ENV), que envolve um dispositivo implantável.
- Escolha do Hospital e Cidade:As despesas cirúrgicas geralmente variam dependendo da cidade e do hospital. Hospitais em cidades metropolitanas como Mumbai ou Bangalore podem cobrar mais do que aqueles em cidades menores.
- Experiência do Cirurgião e Conhecimento da Equipe:Neurocirurgiões altamente experientes e equipes abrangentes de cirurgia de epilepsia normalmente cobram taxas mais altas, o que pode se refletir no custo total do tratamento.
- Testes pré-cirúrgicos e imagens:Antes da cirurgia, os pacientes são submetidos a uma avaliação detalhada que pode incluir exames de ressonância magnética, monitoramento de vídeo EEG, exames PET ou SPECT e avaliações neuropsicológicas. O número e a complexidade destes testes podem impactar significativamente o custo total do tratamento.
- Duração da internação hospitalar e cuidados na UTI:Alguns pacientes podem necessitar de uma internação hospitalar mais prolongada, principalmente aqueles submetidos a procedimentos complexos ou que apresentam complicações pós-cirúrgicas.
- Tipo de Quarto e Alojamento:Quartos privativos, suítes de luxo e comodidades para pacientes, como estadia de acompanhantes ou refeições personalizadas, também podem impactar o custo total.
- Recuperação pós-cirúrgica e medicamentos:As primeiras semanas após a cirurgia podem exigir exames de acompanhamento, medicamentos e reabilitação física ou cognitiva.
Por que escolher a Índia para cirurgia de epilepsia?
A Índia é um centro global para cirurgia de epilepsia, graças à sua combinação única de conhecimento médico, infraestrutura moderna e preços acessíveis. Pacientes de todo o mundo viajam para a Índia todos os anos em busca de cuidados neurológicos avançados que sejam de alta qualidade e com boa relação custo-benefício.
- Neurocirurgiões de classe mundial com treinamento global:A Índia abriga um número crescente de neurocirurgiões altamente treinados, especializados em cirurgia de epilepsia. Eles trazem anos de experiência no tratamento de casos complexos de epilepsia, tanto em adultos como em crianças, e são qualificados em todos os procedimentos relevantes.
- Tecnologia avançada e ferramentas de diagnóstico:Os principais hospitais da Índia estão equipados com as tecnologias mais recentes necessárias para uma cirurgia segura e precisa da epilepsia. Isso inclui ressonância magnética de alta resolução, monitoramento de vídeo EEG, exames PET e SPECT, sistemas de neuronavegação e mapeamento cerebral intraoperatório.
- Altas taxas de sucesso comparáveis às do Ocidente:Os hospitais indianos relatam consistentemente taxas de ausência de convulsões de 60 a 80%, dependendo do procedimento e do perfil do paciente. Além da redução das convulsões, muitos pacientes apresentam melhorias significativas na clareza mental, mobilidade, bem-estar emocional e qualidade de vida geral.
- Pacotes de tratamento econômicos:Uma das razões mais convincentes para escolher a Índia é o custo dramaticamente mais baixo do tratamento. As cirurgias de epilepsia na Índia podem custar 60-80% menos do que nos países ocidentais, sem comprometer a qualidade.
- Cuidado multilíngue e culturalmente sensível:Os hospitais indianos oferecem um ambiente acolhedor e inclusivo para pacientes internacionais. Muitas instituições oferecem intérpretes, pessoal multilingue e cuidados culturalmente sensíveis, garantindo que os pacientes e as suas famílias se sintam compreendidos e respeitados.
- Sem listas de espera e processo simplificado:Ao contrário de muitos países onde os sistemas de saúde públicos envolvem longos tempos de espera, a cirurgia de epilepsia na Índia é agendada prontamente. Depois que o diagnóstico é confirmado e as avaliações pré-cirúrgicas são concluídas, a maioria dos pacientes é submetida à cirurgia em poucos dias.
Serviços para pacientes internacionais
Os principais hospitais e facilitadores de turismo médico da Índia desenvolveram serviços especializados para tornar a cirurgia de epilepsia acessível e sem estresse para pacientes que viajam do exterior. Desde o momento em que o paciente manifesta interesse até muito depois da cirurgia, o sistema é projetado para proporcionar conforto, clareza e conveniência em cada etapa.
- Assistência para Visto Médico:Os hospitais geralmente emitem uma carta-convite para visto, o que ajuda os pacientes a obter um visto médico rapidamente. Em muitos casos, o processamento do visto é acelerado para aqueles que passam por tratamentos neurológicos, especialmente se as convulsões forem frequentes ou alterarem a vida.
- Recolha no aeroporto e transporte local:A maioria dos grandes hospitais oferece serviços de coleta no aeroporto para garantir que os pacientes cheguem com segurança e conforto. O transporte local também é providenciado para visitas de acompanhamento, exames diagnósticos e alta.
- Acomodações e refeições acessíveis:Os pacientes podem escolher entre uma variedade de acomodações próximas, incluindo pousadas e hotéis de luxo. Os serviços de refeições são adaptados às necessidades dietéticas, incluindo opções vegetarianas, halal ou adequadas para diabéticos.
- Serviços de interpretação de idiomas:A comunicação é crucial durante o tratamento. É por isso que os principais hospitais oferecem intérpretes fluentes em árabe, francês, espanhol, russo, suaíli e muito mais, dependendo da região do paciente.
- Coordenadores de pacientes internacionais dedicados:Cada paciente internacional recebe um coordenador que atua como ponto único de contato durante toda a jornada médica. O coordenador ajuda na admissão hospitalar, consultas, faturamento, preparação de documentos e planejamento de alta.
- Cuidados de acompanhamento:Os hospitais costumam agendar teleconsultas depois que o paciente volta para casa para verificar o progresso da recuperação, administrar medicamentos e resolver quaisquer preocupações.
- Suporte para Viagens e Documentação:Os coordenadores de pacientes ajudam com câmbio de moeda, cartas de seguro, extensões de visto e certificados de aptidão para retorno a casa.
Cirurgia de Epilepsia Comparação de custos por país
Compare os custos de Cirurgia de Epilepsia em diferentes países para tomar uma decisão informada sobre o seu tratamento médico.
| País | Faixa de custo (USD) | Poupança potencial | Ação |
|---|---|---|---|
ÍndiaAtualMelhor valor | $4,000 - $9,000 | — | Obter cotação |
Observação: Os custos podem variar de acordo com a escolha do hospital, tipo de quarto, serviços adicionais e requisitos médicos individuais.
Hospitais líderes para Cirurgia de Epilepsia em Índia

Hospital Super Especializado BLK-Max, Nova Delhi
O BLK-Max Super Speciality Hospital em Nova Delhi é uma das principais instituições de saúde da Índia, oferecendo 650 leitos, 22 salas de operações av...
Acreditações


Instalações
Max Smart Super Speciality Hospital, Saket, Nova Delhi
O Max Smart Super Speciality Hospital, Saket, é um hospital terciário com 250 leitos no sul de Delhi. Oferece atendimento médico e cirúrgico avançado ...
Acreditações

Instalações
Hospital PSRI, Delhi
O Instituto de Pesquisa Pushpawati Singhania (Hospital PSRI), em Nova Delhi, é um hospital terciário multiespecializado líder estabelecido em 1996 pel...
Acreditações

Instalações
Procedimentos semelhantes
Galeria

Perguntas frequentes
Autor
Ver tudoDeepanshu Siwach é um farmacêutico clínico experiente com título de Doutor em Farmácia. Ele tem mais de 4 anos de experiência e já trabalhou com milhares de pacientes. Ele está associado a alguns do... Leia mais
Navegar por Departamento
Explore procedimentos em diferentes departamentos
Procedimentos Relacionados
Outros procedimentos neste departamento
Obtenha um plano de tratamento gratuito
Nosso site usa cookies. política de Privacidade.




