Matibabu ya Saratani ya Ngozi Gharama katika India
Kuhusu Matibabu ya Saratani ya Ngozi
Saratani ya ngozi ni miongoni mwa saratani zinazoongezeka kwa kasi duniani kote, zikiathiri laki ya watu kila mwaka. Kulingana na ripoti za afya duniani, zaidi yamilioni 2-3 kesi zisizo za melanomanazaidi ya kesi 130,000 za melanomahugunduliwa kila mwaka, na kuifanya kuwa moja ya aina ya kawaida ya saratani katika vikundi vyote vya umri. Nambari zinazoongezeka zinahusishwa na mambo kama vile kuongezeka kwa mwanga wa jua, kubadilisha mtindo wa maisha, na ufahamu zaidi unaosababisha uchunguzi wa mara kwa mara.
Utambuzi wa mapema huboresha matokeo. Maendeleo ya kisasa ya kimatibabu yamewezesha utambuzi wa haraka wa mabadiliko ya ngozi ya kutiliwa shaka, kuruhusu matibabu yao kwa njia sahihi, zisizo na uvamizi. Leo, aina nyingi za saratani ya ngozi zinaweza kudhibitiwa kwa ufanisi zinapogunduliwa mapema, na kusababisha viwango vya juu vya mafanikio na kupona haraka.
Je! Saratani ya Ngozi ni nini?
Saratani ya ngozi huanza wakati seli zisizo za kawaida kwenye ngozi zinakua na kugawanyika bila kudhibitiwa. Seli hizi huunda misa au kidonda ambacho kinaweza kuonekana kwenye sehemu yoyote ya mwili, pamoja na sehemu ambazo hazipatikani na jua mara kwa mara. Ingawa kesi nyingi hukua polepole, aina zingine hukua kwa ukali zaidi na zinahitaji matibabu ya haraka.
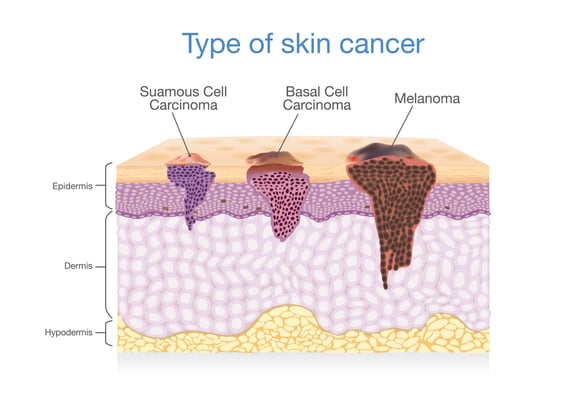
Kuna aina tatu kuu za saratani ya ngozi.
- Basal cell carcinomani ya kawaida na kwa kawaida hukua polepole.
- Squamous cell carcinomakawaida hukua katika maeneo yenye jua na inaweza kuenea ikiwa haijatibiwa.
- Melanomasio kawaida lakini mbaya zaidi kwa sababu inaweza kuenea haraka kwa viungo vingine.
Je! ni Dalili zipi na Saratani ya Ngozi Inatambuliwaje?
Saratani ya ngozi inaweza kuonekana kwa aina nyingi, na ishara za mapema mara nyingi huonekana kuwa hazina madhara. Dalili nyingi huhusisha mabadiliko yanayoonekana kwenye ngozi ambayo yanaendelea, kukua, au kuonekana isiyo ya kawaida ikilinganishwa na maeneo ya jirani.
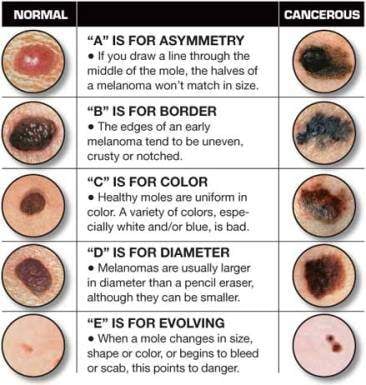
Dalili za kawaida ni pamoja na:
- Doa mpya au ukuaji unaoongezeka polepole kwa ukubwa
- Kidonda kisichopona au kinachoendelea kurudi
- Masi ambayo hubadilika kwa umbo, rangi, au mpaka
- Sehemu ya ngozi ambayo inakuwa mbaya, yenye magamba au yenye ukoko
- Tundu lililoinuliwa ambalo huvuja damu kwa urahisi
- Michirizi ya giza chini ya kucha (katika hali nadra)
Madaktari hugundua saratani ya ngozi kupitia safu ya hatua rahisi na sahihi.
- Auchunguzi wa kliniki wa ngozikwa kawaida ni hatua ya kwanza, ambapo daktari anachunguza mwonekano, umbo, na umbile la kidonda.
- Angozi ya ngozichombo kinaweza kutumika kutazama tabaka za ndani za ngozi kwa uwazi zaidi.
- Ikiwa doa inaonekana kutiliwa shaka, hatua inayofuata nibiopsy, ambapo madaktari huondoa sampuli ndogo ya ngozi na kuichunguza kwa darubini.
- Kwa saratani ya hali ya juu zaidi au zaidi, madaktari wanaweza pia kupendekeza vipimo vya picha, kama vileultrasound,CT scan, auMRI, kuangalia ikiwa saratani imeenea kwa tishu za jirani au nodi za limfu.
Vipimo hivi husaidia kutambua aina, kina, na hatua ya saratani, hivyo kuruhusu madaktari kupanga matibabu kwa usahihi na kujiamini.
Je! Saratani ya Ngozi Inatibiwaje?
Matibabu ya saratani ya ngozi hutofautiana kulingana na aina yake, ukubwa wa ukuaji wake, na ikiwa imebadilika kwa tishu zilizo karibu. Kesi nyingi za hatua za mapema hujibu vyema kwa taratibu rahisi, wakati saratani ya hali ya juu inaweza kuhitaji utunzaji wa kina zaidi.
Kutoboa kwa Upasuaji
Kuondolewa kwa upasuaji ni mojawapo ya matibabu ya kawaida ya saratani ya ngozi. Daktari huondoa doa ya saratani pamoja na ukingo mwembamba wa ngozi yenye afya ili kuhakikisha kibali kamili. Njia hii inafanya kazi vizuri kwa saratani nyingi za basal na seli za squamous.
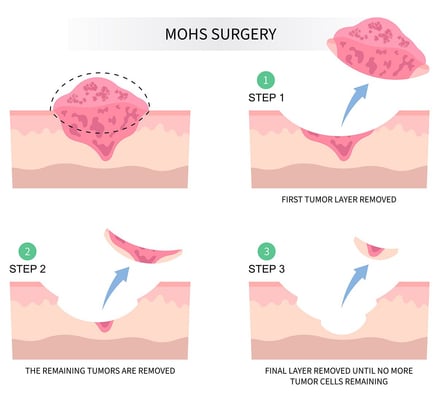
Upasuaji wa Mohs
Upasuaji wa Mohs ni mbinu sahihi, ya safu kwa safu ambayo hutumiwa mara nyingi kutibu saratani kwenye uso au katika maeneo ambayo kuhifadhi mwonekano ni muhimu. Daktari wa upasuaji huondoa safu nyembamba ya tishu za ngozi na kuichunguza mara moja. Hii inaendelea hadi hakuna seli za saratani kubaki. Upasuaji wa Mohs una kiwango cha juu zaidi cha tiba huku ukiokoa ngozi yenye afya iwezekanavyo.
Cryotherapy
Cryotherapy hutumia baridi kali ili kufungia na kuharibu seli zisizo za kawaida. Madaktari hupendekeza hii kwa saratani ya ngozi ya mapema sana au vidonda vya precancerous. Ni haraka, utaratibu rahisi ambao unafanywa kwa msingi wa wagonjwa wa nje.
Tiba ya Mionzi
Tiba ya mionzi inaweza kutumika wakati upasuaji haufai au wakati saratani iko katika eneo dhaifu. Miale inayolengwa huharibu seli za saratani huku ikipunguza uharibifu wa tishu zinazozunguka.
Tiba ya kinga mwilini
Immunotherapy huimarisha uwezo wa asili wa mwili kutambua na kushambulia seli za saratani. Inatumika sana kwa melanoma ya hali ya juu au saratani ambazo hazijibu matibabu ya kawaida.
Tiba inayolengwa
Tiba inayolengwa hufanya kazi kwa kuzuia njia maalum za kijeni au za molekuli ambazo seli za saratani hutumia kukua. Ni ya manufaa kwa watu walio na melanoma ambao wamejua mabadiliko ya maumbile.
Pata mpango wa matibabu ya bure
Kuhusu Matibabu ya Saratani ya Ngozi katika India
Je! Gharama ya Matibabu ya Saratani ya Ngozi nchini India ni Gani?
Gharama ya kutibu saratani ya ngozi nchini India ni kati ya$1,500 hadi $6,000, ambayo ni takriban₹1.2 laki hadi ₹5 laki. Saratani za hatua za awali zinazotibiwa kwa taratibu ndogo hugharimu kidogo, ilhali melanoma ya hali ya juu inayohitaji upasuaji, kinga ya mwili au tiba inayolengwa inaweza kuanguka kwenye ncha ya juu zaidi ya masafa.
Makadirio ya Uchanganuzi wa Gharama:
- Uchimbaji wa upasuaji:₹40,000 – ₹1,00,000
- upasuaji wa Mohs:₹80,000 – ₹1,80,000
- Cryotherapy:₹20,000 - ₹50,000
- Tiba ya mionzi:₹1.5 - ₹3 laki (kulingana na vipindi)
- Tiba ya kinga mwilini:₹1 - ₹2 laki kwa kila mzunguko (inategemea dawa)
- Tiba inayolengwa:Gharama inatofautiana sana kulingana na dawa
Gharama Inajumuisha Nini
Hospitali nyingi zinajumuisha zifuatazo kwenye kifurushi cha matibabu:
- Mashauriano na wataalamu, ikiwa ni pamoja na dermatologists na oncologists.
- Gharama za upasuaji, ikijumuisha ada za upasuaji, ganzi na matumizi ya ukumbi wa upasuaji.
- Matibabu mahususi, ikiwa ni pamoja na kukatwa, upasuaji wa Mohs au cryotherapy.
- Kukaa hospitalini na utunzaji wa uuguzi kwa muda uliopendekezwa wa matibabu.
- Dawa na mavazi hutolewa wakati wa kulazwa hospitalini.
- Ufuatiliaji wa baada ya utaratibu hadi kutokwa, ikiwa ni pamoja na ukaguzi wa jeraha na tathmini muhimu.
Nini Gharama Haijumuishi
Baadhi ya gharama hutoka nje ya kifurushi cha msingi na hutozwa kando:
- Vipimo vya uchunguzi, ikiwa ni pamoja na biopsy, dermoscopy, CT scan, MRI, au PET scan.
- Tiba za hali ya juu, kama vile tiba ya kinga mwilini au dawa zinazolengwa, hutofautiana kwa bei.
- Kukaa hospitalini kwa muda mrefu zaidi ya muda uliopendekezwa kwa sababu ya shida au mahitaji ya juu ya utunzaji.
- Usafiri, visa, na malazi ni gharama za kibinafsi kwa wagonjwa wa kimataifa.
- Urekebishaji maalum, ikiwa inahitajika, baada ya kuondolewa kwa tumor kubwa.
Je, ni Gharama Gani ya Jiji la Matibabu ya Saratani ya Ngozi nchini India?
Gharama ya matibabu ya saratani ya ngozi inatofautiana kidogo kutoka mji mmoja hadi mwingine. Mambo kama vile viwango vya hospitali, upatikanaji wa wataalamu na gharama za afya za eneo huathiri tofauti hizi.
Ifuatayo ni mlinganisho wa takriban ili kuwasaidia wagonjwa kupanga matibabu yao kwa ufanisi zaidi.
Jiji | Gharama ya wastani (USD) | Takriban. Gharama (INR) |
| New Delhi | $1,800 - $5,500 | ₹1,50,000 – ₹4,60,000 |
| Mumbai | $2,000 - $6,000 | ₹1,70,000 – ₹5,00,000 |
| Chennai | $1,600 - $5,000 | ₹1,30,000 – ₹4,10,000 |
| Bangalore | $1,700 - $5,200 | ₹1,40,000 – ₹4,30,000 |
| Hyderabad | $1,600 - $5,000 | ₹1,30,000 – ₹4,10,000 |
Ni Mambo Gani Huathiri Gharama ya Matibabu ya Saratani ya Ngozi nchini India?
Bei ya wastani ya matibabu ya saratani ya ngozi nchini India inatofautiana kwa kila mgonjwa kwa sababu kila kesi ina mahitaji tofauti ya matibabu. Vipengele kadhaa huathiri gharama ya jumla, ikiwa ni pamoja na aina ya saratani, mpango wa matibabu, na huduma za hospitali.
- Aina ya Saratani ya Ngozi:Saratani za basal na squamous cell kawaida huhitaji taratibu rahisi, wakati melanoma mara nyingi huhitaji matibabu ya hali ya juu, ambayo huongeza gharama ya jumla.
- Hatua ya Ugonjwa:Saratani za hatua za awali zinahusisha matibabu ya moja kwa moja, ilhali kesi za hali ya juu zinaweza kuhitaji upasuaji mgumu, matibabu ya muda mrefu, na ufuatiliaji wa karibu.
- Njia ya matibabu inayotumika:Gharama hutofautiana kulingana na ikiwa mgonjwa anahitaji kukatwa, upasuaji wa Mohs, mionzi, tiba inayolengwa, au tiba ya kinga, huku matibabu ya hali ya juu zaidi yakiwekwa bei ya juu.
- Uzoefu wa upasuaji:Wataalamu walio na mafunzo ya kina katika upasuaji wa ngozi au oncologic wanaweza kutoza ada za juu kutokana na utaalamu na usahihi wao.
- Kitengo cha Hospitali:Vituo vya taaluma nyingi vilivyoidhinishwa vilivyo na vifaa vya hali ya juu na vitengo vya oncology kwa ujumla vina gharama ya juu ya matibabu kuliko hospitali za kawaida.
- Uchunguzi wa Utambuzi na Utunzaji wa Ufuatiliaji:Biopsy, uchunguzi wa picha, na ukaguzi unaoendelea huchangia gharama ya jumla, haswa kwa saratani ambazo zinahitaji ufuatiliaji wa muda mrefu.
- Dawa na Msaada wa Msaada:Dawa za baada ya utaratibu, mavazi, na matibabu ya kuunga mkono kwa kiasi kikubwa huathiri gharama ya jumla, hasa kwa wagonjwa wanaofanyiwa matibabu yaliyolengwa au ya kinga.
Je, Gharama ya Matibabu ya Saratani ya Ngozi nchini India Inalinganishwaje na Nchi Nyingine?
Matibabu ya saratani ya ngozi nchini India ni nafuu zaidi kuliko katika mataifa mengi ya Magharibi. Wagonjwa hupokea huduma ya hali ya juu, mbinu za kisasa za upasuaji, na dawa zilizoidhinishwa kimataifa kwa bei ya chini sana, na kuifanya India kuwa mahali pazuri pa wasafiri wa matibabu.
Nchi | Gharama ya wastani (USD) |
| India | $1,500 - $6,000 |
| Marekani | $8,000 - $25,000 |
| Uingereza | $7,000 - $20,000 |
| Thailand | $4,000 - $12,000 |
| UAE | $6,000 - $18,000 |
India inatoa matibabu kwa karibu 70-80% ya bei ya chini huku ikidumisha viwango vinavyolingana na vituo vya kimataifa vya saratani. Hospitali hutumia dawa zilezile zilizoidhinishwa kimataifa na kuzingatia miongozo ya matibabu inayotegemea ushahidi, kuhakikisha utunzaji salama na unaofaa.
Je, ni Kiwango Gani cha Kupona na Kufaulu kwa Matibabu ya Saratani ya Ngozi?
Kupona kwa saratani ya ngozi kunategemea aina ya saratani na njia iliyotumiwa. Kesi nyingi za hatua za awali zinazotibiwa kwa taratibu ndogo hupona haraka, wakati matibabu ya hali ya juu zaidi yanaweza kuhitaji muda mrefu wa kupona na ufuatiliaji unaoendelea.
- Rekodi ya Urejeshaji:Wagonjwa wanaotibiwa kwa kukatwa au kutibiwa kwa njia ya figo kawaida hupona ndani ya siku chache hadi wiki mbili. Taratibu kama vile upasuaji wa Mohs au tiba ya mionzi inaweza kuhitaji muda mrefu wa uponyaji, na matibabu ya hali ya juu ya melanoma yanahitaji ufuatiliaji wa mara kwa mara.
- Kiwango cha Mafanikio:Saratani za ngozi za hatua za awali zina viwango vya juu sana vya mafanikio, mara nyingi zaidi ya 90%, kwa sababu hujibu vizuri kwa matibabu ya wakati. Melanoma ya hali ya juu ina kiwango cha chini cha mafanikio, lakini matibabu ya kisasa kama vile kinga ya mwili na dawa zinazolengwa zimeboresha matokeo kwa kiasi kikubwa.
- Utunzaji wa muda mrefu:Uchunguzi wa mara kwa mara, uchunguzi wa ngozi, na kudumisha tabia nzuri za kulinda jua kuna jukumu muhimu katika kufikia na kudumisha matokeo mazuri, na pia kupunguza hatari ya kujirudia.
Kwa nini Chagua India kwa Matibabu ya Saratani ya Ngozi?
- Miundombinu ya Juu ya Matibabu:Hospitali nchini India zina vitengo vya kisasa vya matibabu ya ngozi, vyumba vya upasuaji vya usahihi wa hali ya juu, na mifumo ya hali ya juu ya kupiga picha ambayo inasaidia utambuzi sahihi na matibabu salama.
- Wataalamu wenye uzoefu:Madaktari wa upasuaji wa ngozi, oncologists, na wataalam wa upasuaji wa Mohs nchini India wana uzoefu mkubwa wa kudhibiti saratani ya ngozi ya kawaida na changamano, kuhakikisha utunzaji unaotegemeka na sahihi.
- Upatikanaji wa Tiba za kisasa:Wagonjwa hunufaika kutokana na njia za hivi punde za matibabu, ikiwa ni pamoja na upasuaji wa Mohs, tiba ya kinga mwilini, na tiba inayolengwa, ambayo hutumiwa duniani kote kwa udhibiti bora wa saratani ya ngozi.
- Huduma ya bei nafuu, ya hali ya juu:India inatoa matibabu ya hali ya juu ya saratani ya ngozi kwa gharama ndogo ya Magharibi. Bei ya chini inaonyesha muundo wa huduma ya afya nchini, si maelewano katika ubora au usalama.
- Hospitali Zilizoidhinishwa:Vituo vingi vya saratani vimeidhinishwa na NABH au JCI, kwa kufuata viwango vikali vya kimataifa vya usafi, usalama, na itifaki za kimatibabu.
- Timu za Matibabu zinazozungumza Kiingereza:Madaktari, wauguzi, na wafanyakazi wa usaidizi huwasiliana vyema kwa Kiingereza, kuhakikisha mchakato wa matibabu unafanyika kwa wagonjwa wa kimataifa.
- Msaada kamili wa mgonjwa:Hospitali hutoa usaidizi wa visa vya matibabu, malazi, uhamisho wa uwanja wa ndege, na uratibu wakati wote wa matibabu, kuhakikisha uzoefu usio na mkazo.
Matibabu ya Saratani ya Ngozi kulinganisha gharama na nchi
Linganisha Matibabu ya Saratani ya Ngozi gharama katika nchi tofauti kufanya uamuzi sahihi juu ya matibabu yako.
| Nchi | Anuwai ya gharama (USD) | Akiba inayowezekana | Hatua |
|---|---|---|---|
IndiaSasaThamani bora | $1,500 - $6,000 | — | Pata nukuu |
Kumbuka: Gharama zinaweza kutofautiana kulingana na uchaguzi wa hospitali, aina ya chumba, huduma za ziada, na mahitaji ya matibabu ya mtu binafsi.
Taratibu zinazofanana
Matunzio

Maswali
Mwandishi
Tazama Zote
Mkuu - Huduma za Wagonjwa wa Kimataifa
Dk. Riya Shree ni mtaalamu wa tiba ya mwili ambaye alimaliza mafunzo yake katika Hospitali ya Mata Chanan Devi, New Delhi, akipata uzoefu wa kuhudumia wagonjwa na urekebishaji. Alihudumu kwenye mstar... Soma zaidi
Vinjari na Idara
Chunguza taratibu katika idara tofauti
Pata mpango wa matibabu ya bure
Tovuti yetu hutumia kuki. Sera ya faragha.
