Bone Marrow Transplant vs CAR-T Cell Therapy: Which Is Better for Blood Cancer?
If you are fighting a blood cancer like leukemia or lymphoma, you have likely reached a crossroad. On one side is the Bone Marrow Transplant (BMT), a proven but intense decades-old treatment. On the other hand, CAR-T Cell Therapy is a groundbreaking 2026 innovation that uses your own immune system to hunt down cancer cells.
Deciding between the two is not about which treatment is better in a laboratory. It is about which one matches your body, your cancer's genetics, and your goals for recovery.
What Is Bone Marrow Transplant And How Does It Work?
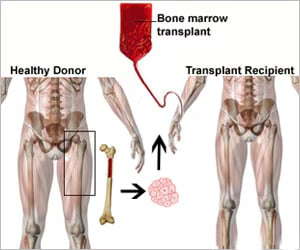
A bone marrow transplant replaces diseased or damaged bone marrow with healthy stem cells. Doctors use this treatment mainly for blood cancers and certain bone marrow disorders.
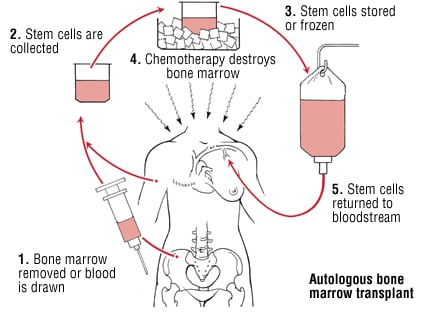
The process begins with high-dose chemotherapy. This step destroys cancer cells and clears space in the bone marrow. Doctors call this phase conditioning therapy.
After conditioning, doctors infuse healthy stem cells into the bloodstream. These cells travel to the marrow and begin producing new blood cells. This process restores the blood-forming system.
There are two main types of transplant. Autologous transplant uses the patient's own stem cells. An allogeneic BMT uses stem cells from a donor. Donor-based transplant can also provide an immune effect that helps attack remaining cancer cells.
What Is CAR-T Cell Therapy And How Does It Work?
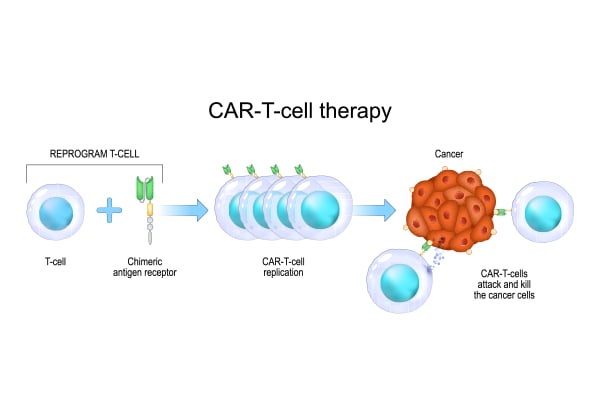
CAR-T cell therapy uses the patient's own immune cells to fight cancer. Doctors modify T-cells in a laboratory to recognize specific cancer markers.
CAR-T cell therapy process begins by collecting T cells from the patient's blood. Scientists then genetically engineer these cells to express a chimeric antigen receptor (CAR). This receptor allows the cells to identify cancer cells more precisely.
After modification, doctors multiply the engineered cells in the laboratory. They then infuse the CAR-T cells back into the patient. These cells search for and destroy cancer cells that carry the target marker.
CAR-T therapy focuses on immune activation rather than bone marrow replacement. The treatment works especially well in certain relapsed leukemias and lymphomas.
Comparing Bone Marrow Transplant and CAR-T Cell Therapy
Choosing between a Bone Marrow Transplant and CAR-T Cell Therapy involves weighing the intensity of the treatment against the precision of the technology. While both aim for a complete cure, their impact on your daily life and your body's recovery timeline differ significantly.
The following table provides a clear comparison to help you discuss these paths with your medical team.
| Feature | Bone Marrow Transplant (BMT) | CAR-T Cell Therapy |
| Primary Mechanism | Total replacement of the blood-forming system. | Genetically re-engineering your own immune cells to hunt cancer. |
| Cell Source | Either your own (Autologous) or a matched donor (Allogeneic). | Exclusively your own T-cells. |
| Treatment Goal | Long-term immune system "reboot" for high-risk or stable disease. | Precision strike for relapsed or treatment-resistant cancers. |
| Hospital Stay | Typically 3 to 4 weeks in a specialized isolation ward. | Typically 1 to 2 weeks for monitoring immune reactions. |
| Major Risk Factor | Graft-versus-Host Disease (GvHD), where donor cells attack the body. | Cytokine Release Syndrome (CRS), a temporary but intense immune response. |
| Recovery Timeline | 6 to 12 months for the immune system to fully mature. | 1 to 3 months for most patients to return to normal activities. |
| Estimated Cost in India | $18,000 to $45,000 (depending on donor and complexity). | $45,000 to $70,000 (reflecting advanced cellular processing). |
Which Conditions Commonly Require Bone Marrow Transplant?
Doctors recommend a bone marrow transplant when blood cancers or marrow disorders carry a high relapse risk. Transplant aims to provide long-term disease control or cure.
- Acute Myeloid Leukemia (AML): High-risk AML often requires allogeneic transplant after remission. Doctors use a transplant to reduce the risk of relapse.
- Acute Lymphoblastic Leukemia (ALL): Adults with high-risk ALL may benefit from a donor transplant. Relapsed ALL also often leads to transplant consideration.
- Multiple Myeloma: Autologous transplant is part of the standard treatment for eligible patients. It extends the duration of remission after initial therapy.
- Aggressive Lymphomas: Relapsed or refractory lymphoma may require a transplant. Doctors use an autologous transplant to consolidate remission.
- Severe Aplastic Anemia and Genetic Blood Disorders: Some non-cancer conditions require a transplant to restore normal blood production. Matched donor transplant offers long-term correction.
Doctors recommend a transplant when the expected benefit outweighs the risk. Careful patient selection improves safety and outcomes.
Which Blood Cancers Benefit From CAR-T Cell Therapy?
CAR-T cell therapy targets specific markers on cancer cells. It benefits selected patients with relapsed or treatment-resistant disease.
- Relapsed or Refractory Acute Lymphoblastic Leukemia: CAR-T therapy has shown strong remission rates in certain pediatric and adult ALL cases. Doctors use it when chemotherapy no longer works.
- Diffuse Large B-Cell Lymphoma: Some aggressive lymphomas respond well to CAR-T after multiple treatment failures. This therapy provides another option when a transplant fails or is not suitable.
- Selected Multiple Myeloma Cases: CAR-T therapy now plays a role in relapsed multiple myeloma. Doctors consider it after standard therapies lose effectiveness.
CAR-T therapy does not suit every patient. Doctors evaluate disease markers, prior treatment response, and overall health before recommending it.
In India, specialized centers offer CAR-T therapy under strict protocols. Careful monitoring supports safety during immune activation.
How Do Success Rates Compare Between Transplant And CAR-T?
Success rates depend on disease type, stage, and prior treatment history. Doctors compare the expected durability of remission and the risk of relapse before recommending either option.
- Bone marrow transplant offers long-term remission in many high-risk leukemias and lymphomas. In selected acute leukemias, donor transplant can provide sustained disease control. The graft-versus-leukemia effect helps eliminate residual cancer cells.
- Autologous transplant in multiple myeloma often extends remission but does not always cure the disease. Patients may still require maintenance therapy after recovery.
- CAR-T cell therapy has shown high initial remission rates in relapsed acute lymphoblastic leukemia and aggressive lymphomas. Some patients achieve rapid and deep responses after infusion. However, durability varies, and relapse can still occur in certain cases.
Doctors evaluate long-term follow-up data carefully. Transplant may provide more durable control in some high-risk diseases. CAR-T therapy offers an important option for relapsed or refractory cases when other treatments fail.
What Are The Risks And Side Effects Of Bone Marrow Transplant?
Bone marrow transplant involves intensive therapy and carries significant risks. Doctors discuss these risks clearly before treatment.
- Infection Risk: High-dose chemotherapy weakens the immune system. Patients remain vulnerable to infection during early recovery. Strict infection control reduces this risk.
- Graft-Versus-Host Disease: In donor transplants, the new immune cells may attack healthy tissue. Doctors use preventive medication to control this reaction. Close monitoring remains essential.
- Organ-Related Effects: Conditioning therapy can affect the liver, lungs, or heart. Doctors perform routine tests to detect early changes. Early intervention improves safety.
- Delayed Blood Count Recovery: Some patients take longer to regain normal blood counts. Extended recovery increases monitoring needs.
- Relapse Risk: Transplant reduces relapse risk but does not eliminate it completely. Ongoing follow-up remains important.
Doctors balance these risks against the potential for cure or long-term remission.
What Are The Risks And Side Effects Of CAR-T Therapy?
CAR-T cell therapy strongly activates the immune system. This activation can cause specific side effects that require close monitoring.
- Cytokine Release Syndrome (CRS): CRS occurs when activated immune cells release large amounts of inflammatory signals. Patients may develop fever, low blood pressure, or breathing difficulty. Doctors monitor closely and use targeted medication to control symptoms.
- Neurological Effects: Some patients develop confusion, headache, or speech difficulty after infusion. Doctors call this immune effector cell–associated neurotoxicity. Most cases improve with supportive care and monitoring.
- Low Blood Counts: CAR-T therapy can temporarily suppress normal blood cell production. Patients may require transfusion support. Recovery usually occurs over time.
- Infection Risk: Immune changes can increase the risk of infection during early recovery. Doctors provide preventive medications and regular follow-up.
CAR-T therapy does not involve marrow replacement, so it avoids graft-versus-host disease. However, immune-related reactions require specialized care during the first few weeks.
How Do Recovery Timelines Differ Between The Two Treatments?
Recovery patterns differ significantly between bone marrow transplant and CAR-T therapy.
- Bone marrow transplant requires a longer initial hospital stay. Patients often remain hospitalized for 3 to 4 weeks. Immune recovery may take several months.
- CAR-T therapy usually involves a shorter hospital admission. Patients often stay for observation during and shortly after infusion. However, close monitoring continues for several weeks.
- Transplant recovery includes gradual rebuilding of the immune system. Doctors monitor blood counts regularly. Patients may need protective isolation during early recovery.
- CAR-T recovery focuses on monitoring immune-related side effects. Most serious reactions occur within the first few weeks. Long-term immune rebuilding remains less intensive than transplant.
How Does Cost Compare Between Bone Marrow Transplant And CAR-T In India?
Costs differ significantly between bone marrow transplant and CAR-T cell therapy in India. The difference mainly reflects laboratory processing, technology, and post-treatment monitoring.
- Bone Marrow Transplant Cost in India: Autologous bone marrow transplant in India usually costs between USD 18,000 and USD 25,000. Allogeneic transplant generally ranges between USD 30,000 and USD 45,000. The total depends on donor type, hospital stay, and complication risk.
- CAR-T Cell Therapy Cost in India: CAR-T cell therapy in India typically costs between USD 45,000 and USD 70,000. The price reflects laboratory modification of immune cells and specialized monitoring. Cost may vary depending on product type and hospital infrastructure.
Transplant often costs less than CAR-T in India. However, a transplant involves a longer hospital stay and prolonged immune recovery. CAR-T therapy may require shorter admission but demands advanced cellular processing.
Cost comparison alone should not guide treatment choice. Disease type, expected response, and long-term benefit remain more important factors.
How Do Doctors Decide Between Transplant And CAR-T Therapy?
Doctors choose between transplant and CAR-T therapy based on disease biology and prior treatment response. Each option serves a different clinical purpose.
- Disease Type and Genetic Risk: Certain leukemias respond better to transplant due to the graft-versus-leukemia effect. Some relapsed lymphomas respond well to CAR-T therapy. Genetic markers guide decision-making.
- Response to Previous Treatment: Patients who relapse after chemotherapy may qualify for CAR-T. Patients who achieve remission but carry a high relapse risk may benefit from BMT.
- Donor Availability: An allogeneic transplant requires a suitable donor. Lack of a donor may shift treatment toward CAR-T when eligible.
- Patient Health and Organ Function: Transplant involves intensive conditioning therapy. Frail patients may tolerate CAR-T better in some cases.
- Long-Term Control Strategy: Transplant often aims for durable remission through immune replacement. CAR-T provides a targeted immune attack without marrow replacement.
Doctors review all factors through multidisciplinary discussion. The goal remains long-term disease control with acceptable risk.
Conclusion
Bone marrow transplant and CAR-T cell therapy both offer advanced treatment for aggressive blood cancers. Transplant provides immune system replacement and long-term disease control in selected cases. CAR-T therapy delivers targeted immune activation in patients with relapsed or resistant disease.
At Qonaq, we see that the decision between BMT and CAR-T is rarely a matter of preference. It is a matter of biology. Doctors evaluate your specific genetic markers, your prior treatment response, and even donor availability.
In India, specialized centers now offer both options under one roof. This allows for a multidisciplinary approach where specialists can determine if CAR-T should be used as a standalone treatment or as a bridge to get you healthy enough for a final transplant. Our goal is to connect you with the teams that prioritize your long-term independence and mobility.
Related Hospitals
Discover hospitals and medical centers related to this topic for quality healthcare services.

MGM Healthcare, Chennai
MGM Healthcare, Chennai, is a 400-bed quaternary-care super-specialty hospital accredited by JCI, NABH, and NABL. The hospital features 100 ICU beds, ...
Accreditations


Facilities

Paras Hospital, Gurgaon
Paras Hospital, Gurgaon, established in 2006, is a 300-bed NABH- and NABL-accredited tertiary care hospital offering over 36 super specialties. The ho...
Accreditations

Facilities

Medanta - The Medicity Hospital, Gurgaon
Medanta – The Medicity in Gurgaon is one of India's largest and most advanced multi-speciality hospitals, founded in 2009 by world-renowned cardiac su...
Accreditations


Facilities

BLK-Max Super Speciality Hospital, New Delhi
BLK-Max Super Speciality Hospital in New Delhi is one of India's premier healthcare institutions, offering 650 beds, 22 advanced operation theatres, a...
Accreditations


Facilities

Max Super Speciality Hospital, Saket, Delhi
Max Super Speciality Hospital, Saket, New Delhi, is a leading JCI- and NABH-accredited hospital offering advanced medical care across 38+ specialities...
Accreditations



Facilities

Fortis Memorial Research Institute (FMRI), Gurgaon
Fortis Memorial Research Institute (FMRI), Gurgaon, is a world-class multi-specialty hospital established in 2013. The hospital offers 330 beds, 15 op...
Accreditations


Facilities
Related Doctors
Connect with experienced doctors and medical specialists in this field.

Dr. Shishir Shetty
Head of Department (HOD)

Dr. Gopal Ramakrishnan
Senior Consultant

Dr. C N Patil
Head of Department (HOD)

Dr. Aditya Murali
Consultant

Dr. Vijay K Ahuja
Senior Consultant

Dr. M S Belliappa
Head of Department (HOD)
Related Articles
Explore more articles and insights on similar health topics.
Back Pain or Something More? When Does a Spine Tumor Require Surgery?

How Long Can You Live After an Organ Transplant?
Who Can Get an Organ Transplant in India? Eligibility Rules Explained
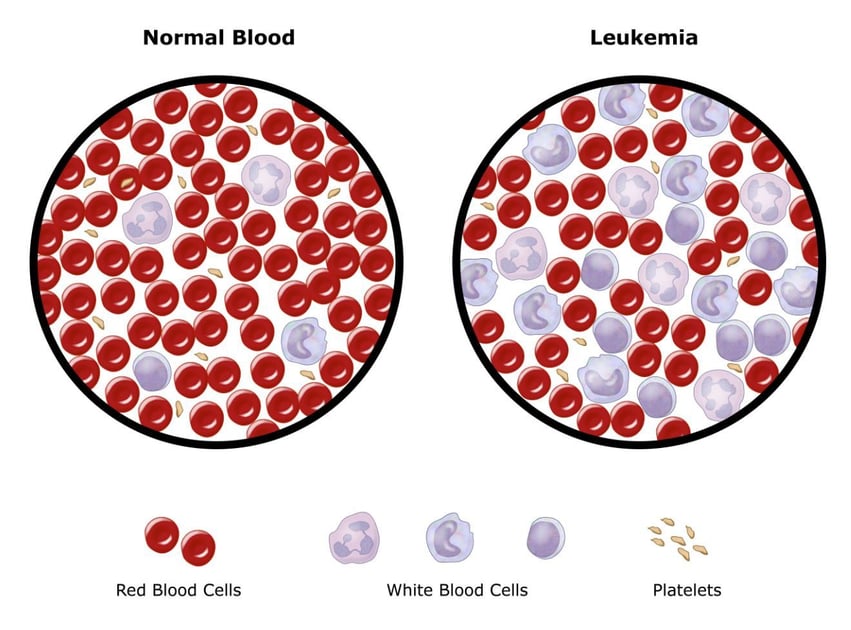
Can You Survive Leukemia Without a Bone Marrow Transplant?
Is Bone Marrow Transplant Worth the Cost? A Financial and Medical Guide for International Patients in India
Is Bone Marrow Transplant Safe for International Patients?
Author
View AllDr. Deepanshu Siwach is an experienced clinical pharmacist with a Doctor of Pharmacy degree. He has over 4 years of experience and has worked with thousands of patients. He has been associated with ... Read More
Our website uses cookies. By clicking on accept you give your consent to the use of cookies as per our Privacy Policy.

