India as a Medical Hub for Patients from Tanzania

Patients from Tanzania increasingly seek medical treatment abroad when serious illness requires faster and more advanced care. Health data shows that non-communicable diseases now cause over40% of deathsin Tanzania, with heart disease, cancer, and kidney failure leading this rise.
Cancer remains a significant concern. Studies indicate that more thantwo-thirds of cancer cases in Tanzaniaare diagnosed at an advanced stage, when treatment becomes urgent and complex. Patients often need immediate access to specialist care and advanced technology.
Geographic distance also affects care. Advanced treatment centers remain limited to a few cities, while most patients live outside these areas. Delays in diagnosis and treatment push families to look beyond national borders.
India has emerged as a practical option for Tanzanian patients seeking timely treatment, experienced specialists, and predictable costs. Many patients begin evaluation and treatment soon after arrival.
For families in Tanzania, medical travel to India represents a step toward faster decisions and complete care when time matters most.
What Healthcare Challenges Do Patients in Tanzania Face?
Patients in Tanzania face healthcare gaps that affect treatment outcomes for serious diseases, especially outside major cities.
- Severe concentration of advanced care in a few urban centers:Most advanced hospitals and specialists operate inDar es Salaam. Patients from regions such as Mwanza, Dodoma, Mbeya, or Arusha often travel long distances for tests or consultations. This travel causes delays, missed follow-ups, and incomplete treatment.
- Limited oncology and radiotherapy capacity:Tanzania has only a few radiotherapy units for a population of over 65 million. Cancer patients often wait weeks for imaging, biopsy confirmation, or treatment slots. Late diagnosis combined with treatment delay reduces survival chances.
- Shortage of specialist doctors for complex diseases:Specialists in cardiothoracic surgery, neurosurgery, oncology, transplant medicine, and interventional cardiology remain limited. Many patients receive only initial stabilization before referral abroad.
- Delayed diagnosis of chronic diseases:Conditions such as heart disease, kidney failure, and diabetes often remain undetected until advanced stages. Limited access to advanced imaging, cardiac testing, and nephrology services contributes to late presentation.
- High out-of-pocket spending with incomplete care:Most patients pay for private healthcare directly. Even after spending large amounts, families may still not receive complete treatment. It pushes them to seek destinations where a single system manages diagnosis, treatment, and follow-up.
What Cultural and Practical Factors Connect Tanzania with India?
Patients from Tanzania often choose India because the treatment experience aligns well with language comfort, family involvement, and financial planning.
- Comfort with English-based medical communication:English serves as the primary language of education and healthcare in Tanzania. Indian doctors explain medical conditions and treatment plans clearly in English, reducing misunderstandings and building trust.
- Strong acceptance of family-supported care:Tanzanian patients usually travel with a close family member. Indian hospitals support family presence during consultations and recovery, which aligns with Tanzanian cultural expectations for caregiving and decision-making.
- Long-standing East Africa–India connection:India has a long history of educational, trade, and medical links with East Africa. Many Tanzanian families already view India as a familiar and reliable country for professional services, including healthcare.
- Affordability for self-funded treatment:Most Tanzanian patients rely on savings rather than insurance. India offers advanced care at costs that remain manageable for middle-income families, even for long treatments like cancer therapy or surgery with rehabilitation.
- Practical living conditions during extended stays:Medical treatment often requires weeks of stay. India offers flexible accommodation, affordable daily living costs, and access to medicines, which helps families manage extended treatment periods.
Why Do Patients from Tanzania Prefer India for Medical Care?
- Faster decision-making for time-sensitive illnesses:Many Tanzanian patients reach hospitals only after symptoms have persisted for months. India offers rapid scheduling for imaging, biopsy, and surgery. Patients often complete evaluation and start treatment within days, which matters for cancer, heart disease, and kidney failure.
- Depth of specialist experience for complex cases:Indian doctors manage very high volumes of advanced cases every year. Tanzanian families often choose India because specialists regularly handle late-stage cancers, complex cardiac disease, and revision orthopedic surgery.
- Clear treatment plans for self-funded patients:Most patients from Tanzania pay out of pocket. Indian hospitals share step-by-step treatment plans with cost estimates early.
- Continuity of care in one system:Patients receive diagnosis, treatment, rehabilitation, and follow-up in one coordinated pathway. This continuity reduces the need for multiple referrals and repeated travel.
What Treatments Do Patients from Tanzania Commonly Seek in India?
Patients from Tanzania travel to India mainly for treatments that require advanced technology, specialist depth, and long-term planning.
- Cancer diagnosis and comprehensive cancer treatment:Common reasons include breast, cervical, prostate, colorectal, and blood cancers. Patients value access to imaging, biopsy, surgery, chemotherapy, and radiation in one coordinated plan, especially after a late diagnosis at home.
- Heart disease and cardiac surgery:Patients seek bypass surgery, valve repair or replacement, angioplasty, and advanced cardiac evaluation. Indian cardiac centers manage high-risk and late-presenting cases with structured recovery plans.
- Kidney disease care and transplant evaluation:Chronic kidney disease leads many patients to seek dialysis planning and kidney transplant assessment. Indian centers provide organized pathways and clear long-term follow-up guidance.
- Orthopedic surgery and joint replacement:Total knee and hip replacement attract patients with advanced arthritis or untreated joint damage. Predictable recovery timelines and rehabilitation support help patients return home safely.
- Spine surgery and neurology care:Patients seek treatment for slipped discs, spinal stenosis, nerve compression, and brain tumors. Access to advanced imaging and minimally invasive techniques drives these choices.
- Fertility treatment and women's health care:Couples travel for IVF, ICSI, and advanced fertility testing. Transparent planning and affordability compared with Western options support continued treatment.
What Is the Cost of Treatment in India for Patients from Tanzania?
Costs strongly shape patients' decisions in Tanzania, as most families pay out of their own savings. India offers advanced treatment at prices that fit this reality and allow patients to complete full care, not partial treatment.
- Upfront estimates before travel:Indian hospitals usually review reports and share cost ranges before admission. It helps Tanzanian families decide early and plan travel, stay length, and finances without uncertainty.
- Lower overall cost of complex care:Even when patients arrive with advanced disease, India keeps costs far lower than those in Europe or the Middle East.
Approximate Treatment Costs in India
- Total Knee Replacement (TKR):USD 4,000 – 5,500
- Total Hip Replacement (THR):USD 4,500 – 6,000
- Heart Valve Replacement:USD 6,000 – 9,000
- Bypass Surgery (CABG):USD 3,500 – 6,000
- Kidney Transplant:USD 13,000 – 15,000
- Advanced dialysis planning:significantly lower than regional private options
- Ovarian Cancer Treatment:USD 3,800 – 8,000
- Lung Cancer Treatment: USD 4,500 – 8,500
- Cervical Cancer Treatment: USD 2,500 – 7,500
- Prostate Cancer Treatment: USD 3,000 – 10,000
- Breast Cancer Treatment: USD 2,500 – 12,000
Lower medical bills, affordable medicines, and reasonable living costs during extended stays help families finish treatment without financial collapse.
How Does Treatment Cost in India Compare with Other Countries for Patients from Tanzania?
Patients from Tanzania commonly compare India with South Africa, Turkey, Europe, and the Gulf before choosing where to go.
- South Africa:Advanced care is available, but private treatment remains expensive. Hospital charges and long stays increase total expenses. Many Tanzanian families find India more affordable with faster access to healthcare.
- Turkey:Turkey attracts some East African patients, but prices for joint replacement, cardiac surgery, and cancer care are often much higher than in India. Living costs during long treatment add further burden.
- Europe and the Gulf:These regions provide high-quality care but remain financially out of reach for most Tanzanian families. Insurance coverage rarely applies, and waiting times can be long.
Treatment Type | South Africa / Turkey (USD) | Europe / Gulf (USD) | India (USD) |
| Total Knee Replacement | 18,000 – 30,000 | 30,000 – 45,000 | 4,000 – 5,500 |
| Total Hip Replacement | 20,000 – 35,000 | 35,000 – 50,000 | 4,500 – 6,000 |
| Heart Valve Replacement | 25,000 – 45,000 | 60,000 – 90,000 | 6,000 – 9,000 |
| Kidney Transplant | 70,000 – 120,000 | 150,000 – 200,000 | 13,000 – 15,000 |
| Cancer Treatment (full cycle) | 30,000 – 60,000 | 50,000 – 100,000 | 8,000 – 12,000 |
How Easy Is Travel from Tanzania to India for Medical Treatment?
Patients from Tanzania usually plan travel with medical urgency and family support in mind. India offers routes and on-ground coordination that suit these needs.
Travel commonly routes throughAddis Ababa, Doha, Dubai, or Nairobito major Indian cities. Flight time typically ranges from8 to 12 hours, depending on connections. These hubs regularly handle medical travelers, which keeps transit predictable.
- Entry through major medical hubs in India:Cities such as Delhi, Mumbai, and Chennai receive a high volume of international patients. Airport procedures remain structured, which helps patients arriving tired or unwell.
- Arrival assistance and hospital coordination:Hospitals often arrange airport pickup and direct transfer to accommodation or the hospital. This support reduces stress after long flights and helps avoid navigation issues in unfamiliar areas.
- Pre-travel planning support:Patients usually receive guidance on flight timing, transit requirements, and arrival schedules. Clear planning helps families manage documents, medicines, and rest periods.
Overall, travel from Tanzania to India remains manageable and well-organized for medical purposes, especially with prior coordination.
What Is the Success Rate of Medical Treatment in India for Patients from Tanzania?
Success rates matter because many Tanzanian patients arrive with advanced disease after a delayed diagnosis. India reports strong outcomes across major procedures, driven by experience with high-risk cases and structured follow-up.
- Total Knee Replacement (TKR):Most patients achieve durable pain relief and improved mobility. Reported success rates range between95% and 98%with proper rehabilitation.
- Total Hip Replacement (THR):Long-term outcomes remain strong, with success rates typically95%–98%, even in complex cases.
- Heart surgery (bypass and valve procedures):High-volume centers report success rates of94%–97%, depending on heart function and overall health at presentation.
- Kidney transplant:One-year graft survival generally ranges between90% and 95%. Care teams emphasize medication adherence and follow-up before patients return home.
- Liver transplant:Short-term success rates usually range from85% to 90%for appropriately selected patients, supported by structured post-transplant care.
- Cancer treatment outcomes:Results vary by cancer type and stage. Early-stage cancers show high control and remission rates. Multimodal treatment improves outcomes for advanced disease.
How Can Patients from Tanzania Get an Indian Medical Visa for Treatment?
Patients from Tanzania usually plan medical travel carefully because treatment often involves family savings and extended stays. India offers a clear and practical medical visa process that supports this journey.
- Indian Medical Visa (MED Visa):Patients apply for a Medical Visa explicitly issued for treatment. This visa allows entry for diagnosis, surgery, therapy, and recovery. It also supports multiple entries when follow-up visits are required.
- Visa duration suitable for long-term treatment:Medical visas are generally issued for up toone year, depending on the treatment plan. This duration suits cancer therapy, cardiac recovery, and rehabilitation without pressure to exit early.
- Medical Attendant Visa for family members:Most Tanzanian patients travel with a close relative. India issues Medical Attendant Visas so family members can stay throughout treatment and recovery, which matches family-centered care practices.
- Processing time for Tanzanian applicants:Once documents are complete, processing usually takes2 to 4 working days. Hospitals provide visa invitation letters (VILs) to expedite approval and avoid delays.
Documents commonly required
- Valid Tanzanian passport
- Recent passport-size photographs
- Medical reports from a hospital or doctor in Tanzania
- Treatment or invitation letter from an Indian hospital
- Proof of funds for treatment and stay
- Completed medical visa application form
Overview
Patients from Tanzania choose India for advanced medical care that remains affordable and accessible. Treatment starts quickly, specialists manage complex cases daily, and outcomes remain strong. Precise planning and family support reduce stress. This balance makes India a dependable destination for serious medical treatment.
មន្ទីរពេទ្យពាក់ព័ន្ធ
ស្វែងរកមន្ទីរពេទ្យនិងមណ្ឌលសុខភាពទាក់ទងនឹងប្រធានបទនេះសម្រាប់សេវាកម្មថែទាំសុខភាពដែលមានគុណភាព។

ឧទ្យានវេជ្ជសាស្ត្រ Bahcelievler មន្ទីរពេទ្យ
Medical Park Bahcelievler Hospital គឺជាមន្ទីរពេទ្យដែលមានការទទួលស្គាល់ពី JCI ដែលមានគ្រែ 242 នៅទីក្រុងអ៊ីស្តង់ប៊ុល ដែលបានបង្កើតឡើងក្នុងឆ្នាំ 2007។ លាតសន...
ការទទួលស្គាល់

មធ្យោបាយបរិក្ខារ

មន្ទីរពេទ្យឯកទេស BLK-Max ទីក្រុងញូវដេលី
មន្ទីរពេទ្យ BLK-Max Super Specialty Hospital នៅទីក្រុងញូវដេលី គឺជាស្ថាប័នថែទាំសុខភាពលំដាប់កំពូលមួយរបស់ប្រទេសឥណ្ឌា ដែលផ្តល់ជូននូវគ្រែចំនួន 650 រោងមហោស្...
ការទទួលស្គាល់


មធ្យោបាយបរិក្ខារ

វិទ្យាស្ថានស្រាវជ្រាវ Fortis Memorial (FMRI), Gurgaon
វិទ្យាស្ថានស្រាវជ្រាវ Fortis Memorial (FMRI) Gurgaon គឺជាមន្ទីរពេទ្យពហុឯកទេសលំដាប់ពិភពលោកដែលត្រូវបានបង្កើតឡើងក្នុងឆ្នាំ 2013។ មន្ទីរពេទ្យផ្តល់ជូនគ្រែច...
ការទទួលស្គាល់


មធ្យោបាយបរិក្ខារ

មន្ទីរពេទ្យ Artemis, Gurgaon
មន្ទីរពេទ្យ Artemis, Gurgaon គឺជាមន្ទីរពេទ្យពហុឯកទេសដែលត្រូវបានទទួលស្គាល់ដោយ JCI ដែលត្រូវបានបង្កើតឡើងក្នុងឆ្នាំ 2007 ។ វាផ្តល់ជូននូវគ្រែចំនួន 750+ និង...
ការទទួលស្គាល់



មធ្យោបាយបរិក្ខារ

មន្ទីរពេទ្យ Kokilaben Dhirubhai Ambani ទីក្រុងបុមបៃ
មន្ទីរពេទ្យ Kokilaben Dhirubhai Ambani ក្រុង Mumbai គឺជាមន្ទីរពេទ្យថែទាំសុខភាពប្រចាំត្រីមាសដែលត្រូវបានទទួលស្គាល់ដោយ JCI, NABH, NABL និង CAP ដែលបានបង្ក...
ការទទួលស្គាល់



មធ្យោបាយបរិក្ខារ

មន្ទីរពេទ្យ Medicover, Hitech City, Hyderabad
មន្ទីរពេទ្យ Medicover, Hitech City, Hyderabad គឺជាមន្ទីរពេទ្យទំនើបពិសេសដែលទទួលស្គាល់ដោយ NABH ដែលមានគ្រែចំនួន 400 ដែលបានបង្កើតឡើងក្នុងឆ្នាំ 2011។ វាគឺជ...
ការទទួលស្គាល់


មធ្យោបាយបរិក្ខារ
គ្រូពេទ្យដែលពាក់ព័ន្ធ
ភ្ជាប់ទំនាក់ទំនងជាមួយវេជ្ជបណ្ឌិតដែលមានបទពិសោធន៍និងអ្នកឯកទេសខាងវេជ្ជសាស្ត្រក្នុងវិស័យនេះ។

វេជ្ជបណ្ឌិត Dilek Benk Silfeler
Consultant

លោកបណ្ឌិត Ananda Mandal
Consultant

បណ្ឌិត Indranil Khan
Consultant

បណ្ឌិត Pradip Chakrabarti
Head of Department (HOD)

វេជ្ជបណ្ឌិត Rakesh Rajput
Head of Department (HOD)

បណ្ឌិត Chandramohan K
Senior Consultant
អត្ថបទពាក់ព័ន្ធ
ស្វែងរកអត្ថបទនិងការយល់ដឹងបន្ថែមលើប្រធានបទសុខភាពប្រហាក់ប្រហែល។
តើវាមានគ្រោះថ្នាក់ក្នុងការពន្យារពេលការវះកាត់ឆ្អឹងខ្នងទេ?
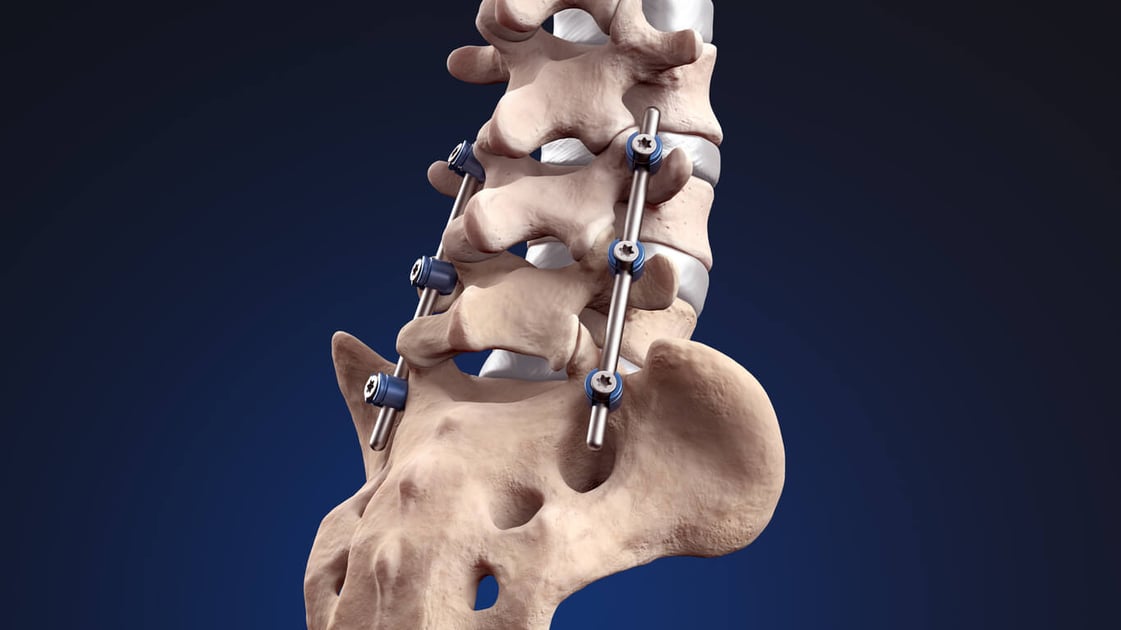
តើនៅពេលណាដែលអ្នកគួរពិចារណាការវះកាត់សម្រាប់ឌីស Herniated?
ការច្នៃប្រឌិតថ្មីបំផុតក្នុងការវះកាត់ខួរក្បាល និងឆ្អឹងខ្នង
តើអ្វីជាអត្រាជោគជ័យពិតប្រាកដនៃការវះកាត់ឆ្អឹងខ្នង?
តើការវះកាត់ឆ្អឹងខ្នងនៅក្រៅប្រទេសមានសុវត្ថិភាពទេ?
របៀបរៀបចំសម្រាប់ការប្តូរសរីរាង្គនៅក្រៅប្រទេស៖ បញ្ជីពិនិត្យសុខភាព ច្បាប់ និងការធ្វើដំណើរ
អ្នកនិបន្ធ
មើលទាំងអស់វេជ្ជបណ្ឌិត Deepanshu Siwach គឺជាឱសថការីគ្លីនិកដែលមានបទពិសោធន៍ដែលមានសញ្ញាបត្របណ្ឌិតផ្នែកឱសថសាស្រ្ត។ គាត់មានបទពិសោធន៍ជាង 4 ឆ្នាំ និងបានធ្វើការជាមួយអ្នកជំងឺរាប់ពាន់នាក់។ គាត់ត្រូវបានផ្សារភ្ជាប់ជាមួយនឹ... អានបន្ថែម
គេហទំព័ររបស់យើងប្រើខូឃីស៍។ គោលការណ៍ភាពឯកជន.

